Dissemination and communication
Good dissemination and communication needs to be a carefully planned process
Dissemination and communication
Dissemination is the targeted distribution of information and materials about an evidence-based intervention to a specific public health or clinical practice audience (AHRQ 2012). For public health more specifically, health communication ‘aims to change people’s knowledge, attitudes, and/or behaviours [and] empower individuals to change or improve their health conditions.’ (Rural Health Information Hub, 2019)
Well-designed dissemination strategies can improve access to a guideline and lead to improvement in health outcomes (Grimshaw, Thomas et al. 2004; Flodgren, Hall et al. 2016). Good dissemination and communication needs to be a carefully planned process that involves considering the target audience, the message you want to get across and the communication strategies that will help you achieve this (Wilson, Petticrew et al. 2010). It also involves consumers whose knowledge and lived experience are critical in the planning stages for dissemination and communication.
Another important and necessary consideration is the political context and any potential impact on the government — a key stakeholder — by a possible counter-campaign if the guidelines address a sensitive health issue.
This module focuses on planning for both activities and the strategies you can use. A similar planning process, discussed below, can be used for both but will need to take into account the different settings, target audiences and key messages.
Other modules you might find useful include the Implementability, Implementation, Engaging stakeholders and Consumer involvement modules.
What to do
1. Plan for dissemination
There are many ways to plan for the dissemination of your guideline such as those described in the Agency for Healthcare Research and Quality (AHRQ) Dissemination planning tool (2005) and the GIN Dissemination of guidelines.
The development of a plan can run through the following stages of a cycle, as outlined in the figure below.
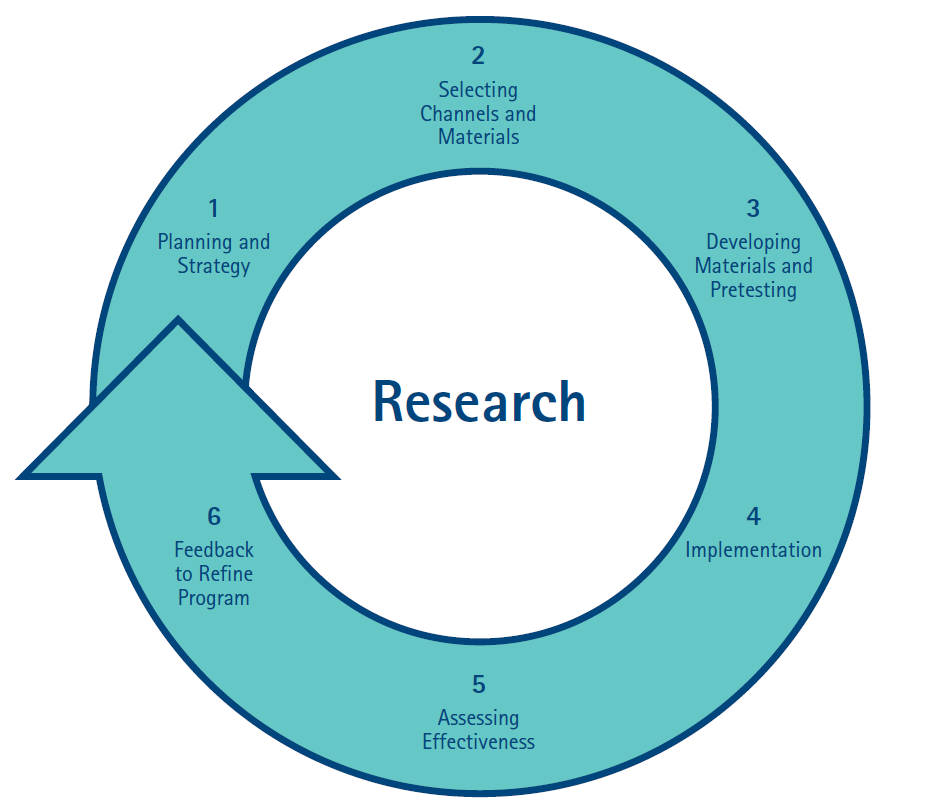
From: ‘The Social Marketing Wheel’, National Cancer Institute, in National Institute for Health Care Management Foundation Issue Brief March 2009
Using the cycle as a guide, a plan will typically contain the following elements:
Research
Research that informs the strategy, such as the systemic review undertaken for the development of the guidelines, a review of previous successful campaigns and identifying your audience information needs.
Planning
- dissemination objectives
- target audience — identifying who they are, what their current perceptions are, what their preferred way of receiving information is
- key messages, including the ‘call to action’ message, and any messages to counter negative campaigns by potential interest groups
- work plan, including activities, source/channel, timeframe, responsibilities, budget
Selecting channels and materials
- dissemination options
- a list of appropriate materials, which should be pre-tested in focus groups
- a stakeholder list with details of who you are going to notify
Assessing effectiveness and refining the program
- a plan for evaluating the effectiveness of the dissemination
- a plan to manage ongoing changes to the guideline and associated dissemination strategy.
A structured and detailed plan should account for all the steps outlined in this module. An example of a template that you can use to help prepare a dissemination plan is at Appendix 1.
The case study below outlines the public health communication strategy behind Australia’s 1997 smoking cessation campaign, which reflects many of these stages.
Australia’s National Tobacco Campaign: Every cigarette is doing you damage
Australia’s National Tobacco Campaign, Every cigarette is doing you damage, led by the Commonwealth in collaboration with the states and territories, was launched in 1997. The strategy was based on expert advice from the Health Minister’s Ministerial Tobacco Advisory Group.
The research base for the communication strategy included a review of forty years of psychological research, as well as a review of reports that had been commissioned and evaluated by Quitlines over the previous decade. The Advisory Group recommended that the campaign target smokers aged between 18 to 40, with messages focused on the positive reasons to quit, being supportive of efforts to quit, as well as discouraging uptake. Advertising had a lower socioeconomic bias to ‘reflect the social class gradient of smoking’. The campaign also had a brief to elevate quitting to a more immediate, actionable place on people’s personal agenda.
Specialists in cardio-vascular, respiratory and neurology provided expertise on the development of the messaging, research data and advice on clinical aspects of disease. They also acted as spokespeople for the campaign.
Two working groups were created — a GP working group made up of representatives from the RACGP, AMA and the Divisions of GP, to promote the campaign among GPs; and a pharmacy working group, which developed a nicotine replacement therapy (NRT) kit for pharmacists, based on evidence reporting the efficacy of NRT.
The campaign also developed strategic relationships with various health sector organisations to reinforce the credibility of the campaign and to provide wider access to the target group.
Media included TV and radio; outdoor advertising such as billboards, public transport and supermarket trolleys; a website; and print materials for GPs and pharmacists. Information was also channelled through Quitline networks in each state and territory, as well as other partnerships. Quitlines were provided with additional funding to increase their training and capacity to respond.
A separate media strategy for people from a non-English speaking background was also developed, based on understanding the social and cultural aspects of smoking in each community. It incorporated the use of ethnic radio and press, workplace initiatives, GPs and bilingual health workers.
The evaluation of the first phase of the campaign — a six-month period from its launch — showed that the campaign ‘evoked a reaction from smokers at a level unsurpassed by [previous campaigns]’ and identified insights that were used to ‘build on the effectiveness of the strategy’ to continue to reduce smoking prevalence.
Every cigarette is doing you damage was critically acclaimed, and has since been used in the United States, British Columbia, New Zealand and Singapore.
From: http://webarchive.nla.gov.au/gov/20140801095025/http://www.health.gov.au/internet/main/publishing.nsf/Content/health-pubhlth-publicat-document-metadata-tobccamp.htm
It’s a good idea to review information from any stakeholder consultation process to help develop a dissemination strategy. Involving consumers and other stakeholders in the dissemination planning process, as well as the guideline development phase will help you make sure that the format and language of any products is appropriate, useful and accessible (see the Consumer involvement and Engaging stakeholders modules). Consumers can also help you identify opportunities for promoting the guideline, or identify potentially negative attention.
Proactively consider the political context. This is a crucial step at this point in the planning phase. If the health issue is likely to attract negative attention, and possibly impact the government, you will need to purchase professional media advice. A professional service will help you plan for, and respond to, any negative counter-campaigns; identify key spokespeople; and help you brief the appropriate minister as part of your dissemination strategy.
You will also need to budget for any activities identified in the strategy (see the Project planning module). Depending on your resources, you may consider hiring media or communications experts to help you with the communication activities and a strategy to notify journalists if appropriate. Digital technical experts may also need to be budgeted for depending on what digital media you use to disseminate your guideline and key messages.
Some parts of your plan — such as budgeting — can be included in your guideline project plan (see the Project planning module). However, the dissemination plan or communication strategy is typically a stand-alone document that accompanies the final guideline. You might like to consider releasing your dissemination plan for public consultation along with your draft guideline. This will allow you to gain feedback from end users about preferred methods of dissemination and help to identify any other channels or opportunities for dissemination that you might have missed.
2. Consider your target audience
It is important for you to consider who will be affected by your guideline and its recommendations, or who will use it and in what health settings. These groups will be your target audience. Target audiences for public health and environmental health guidelines can be very different to clinical practice guidelines and will often include local, state and federal government agencies, and the public. You may have already defined these groups when you scoped your guideline or planned for stakeholder and consumer engagement (see the Scoping the guideline, Consumer involvement and Engaging stakeholders modules); but it is now important to revisit that information to understand their information needs and preferences.
If your guidelines seek to change the behaviours of the public, you may need to consider where your target audience sits along a ‘process of behaviour change’ (PBC) spectrum (Piotrow et al, quoted in O’Sullivan et al, 2003, p8). The PBC describes a spectrum of behavioural change from pre-knowledgeable — where the audience is unaware of the problem or personal risk — to advocating and practising the desired behaviours. Where your target audience sit along this spectrum will help you to tailor your messaging and media more effectively to different ‘segments’.
Conducting a communication needs assessment of these segments will help you tailor your dissemination strategy towards their particular requirements, for example, the Canadian Stroke Best Practice Recommendations 7th Edition (Schipper, Bakker et al. 2016). Involving consumers is useful at this stage as they can provide advice on their experiences with the health care system and will also know where to access this information.
Consumers will also be important in developing key messages.
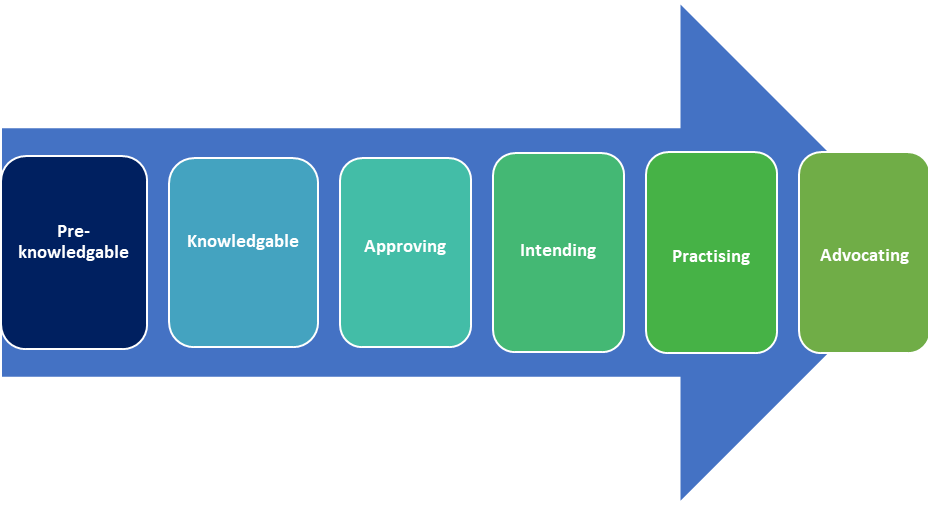
From: Process of change, adapted from Piotrow et al, 1997 in O’Sullivan et al, 2003, p8
3. Select key messages
Messages should be direct, simple, clear, action-oriented (a clear ‘call to action’), concise and consistent (Wilson et al, 2010). They should also take into account the audience’s needs and abilities with respect to the evidence (WHO 2014). If possible, these messages should be brief — a member of this audience should be able to read, watch, or listen to their key messages in two minutes or less. See the AHRQ’s Dissemination Planning Tool (2005).
Using plain language is essential for any dissemination aids for people who have an interest in the guideline but who may not be the ones carrying out the recommendations. For example, guidelines on water quality aimed at local health authorities and regulators need to have technical key recommendations, but also plain language messages for the public to use in advocacy or promotion activities. The type of platform used to disseminate a message will also affect the type of language used. For example, information sent via email may allow the use of more technical language, whereas the same information sent out on social media will use different vocabulary.
Although the development of a standardised language that can explain scientific evidence is an ongoing effort (Langendam, Akl et al. 2013), for example, the Australian Government Writing Guide or NICE Rules for clear writing, as a general rule use less medical and technical terms or give a brief explanation of any terms you can’t avoid (Schipper, Bakker et al. 2016). Also, a guideline written in plain language will make developing dissemination materials easier.
Additionally, different target audiences may be interested in different recommendations, so you will need to tailor the content of material to reflect this. For example, in relation to guidelines on chronic obstructive pulmonary disease (COPD), nurses were interested in recommendations related to health promotion and patient education around early recognition of COPD; whereas GPs were interested in recommendations relating to the treatment of depression in these patients. Their differing interests will affect content, format and dissemination. (Yawn, Akl et al. 2012).
4. Consider dissemination options
There will be a range of options to reach different target audiences (Grimshaw, Eccles et al. 2006; Gagliardi, Marshall et al. 2015; Schipper, Bakker et al. 2016), which are outlined in Table 1.
Proactive dissemination methods such as education campaigns, face-to-face workshops or social marketing campaigns are better than passive dissemination strategies, such as leaflet or brochure campaigns. Evidence though, suggests that using a combined dissemination approach is more effective than using a single approach (Grimshaw, Schunemann et al. 2012; Schipper, Bakker et al. 2016) (Grimshaw, Shirran et al. 2001). Traditional options will usually require higher amounts allocated to them in the budget.
Even so, if you decide to use social media to reach certain demographics, you will need to consider which social media platform is best to use, what you want to communicate and what you would like the recipient to do with that information (‘the call to action’). By its nature, social media is designed to elicit quick responses and create a two-way dialogue between yourselves and the audience. With this in mind, the budget will need to incorporate someone to monitor your messaging.
There are a number of ways to get your message across to your end users:
- identify people or organisations who will help spread the word about your guidelines
- invite your guideline development group members, related organisations and advocacy groups to contribute to dissemination (Gupta, Licskai et al. 2013)
- ask the consumer members of your guideline development group if they can help promote the guideline through their networks or by presenting at conferences (see the Consumer involvement module)
- consider advocacy and special interest groups who may have a regular newsletter or social media page to reach their members.
Consider posting your guideline on databases that have large followings such as the Guideline International Network guidelines database.
Make good use of your networks and connections through your guideline development group members, consumer networks and endorsing organisations. (See the Canadian Stroke Best Practice Recommendations 7th Edition) Build partnerships with professional organisations because endorsement from professional organisations can be helpful for you to disseminate and increase the uptake of guidelines among some user groups. Make sure you check their endorsement policy and the review processes of these organisations carefully, together with any associated costs before submitting your guideline.
The Kidney Health Australia — Caring for Australasians with Renal Impairment (KHA-CARI) Guidelines
A summary of dissemination activities for clinicians and people living with renal impairment:
- publication — summary guidelines in Nephrology
- website — posting all summary and complete guidelines
- nephrologists provided with links to electronic version of all guidelines via electronic newsletter
- electronic version of the complete guidelines sent to all Australian and New Zealand renal units using USB memory cards
- promotion of access to the guidelines through website and news and events (presentation, conferences, publications)
- e-bulletins, email campaigns, newsletters to consumers, for example, through the Kidney Health Australia network or medical institutes.
Table 1: Examples of dissemination options for different audiences
| Dissemination options | Reach to target audience | ||
|---|---|---|---|
| Consumers and the general public | Healthcare Professionals | Other stakeholders (e.g. local government authorities, industry bodies, policymakers) | |
| Official Launch/Launch event | |||
| Press release | O | O | O |
| Web resources release | O | O | O |
| Marketing | |||
| Mass media campaign | O | O | O |
| Social media marketing | O | O | O |
| E-mail distribution | O | O | O |
| Reminders | O | O | |
| Workshop/meetings | |||
| Workshop/Seminar or meeting | O | O | O |
| Webinar | O | O | O |
| Use your networks | |||
| Contact network, opinion leader, champion | O | O | O |
| Register on guideline databases | O | ||
| Endorsement from related organisations | O | O | |
| Journal Publication | O | ||
5. Develop appropriate materials
For healthcare professionals the most common dissemination strategy involves distribution of educational materials; however, this might not always be the best option for reaching your target audience. The different needs of your target audiences will mean that you will have to develop or adapt materials that are appropriate for each audience segment while ensuring the key messages are maintained and consistent between formats. ‘Questions and Answers’ and ‘Frequently Asked Questions’ resources can be particularly helpful, especially for public health advice and guidelines. Involvement of consumers, through focus groups or workshops is critical in this process. Consultation with state and territory health departments can also be effective, for example, see NHMRC’s 2017 Public statement — water fluoridation and human health.
Obtain legal advice on potential copyright issues for any proprietary products that might be produced. Also consider translating any products to multiple languages or assisted technology, using National Accreditation Authority for Translators and Interpreters accredited services (WHO 2014). This is especially important if your recommendations affect sectors of the community that do not use English as their primary language.
6. Consider other ways to improve accessibility
End users will need to easily access your guideline and related material and so you will need to consider how end users will actually find your guideline. For example, people will be less likely to read your guideline if it is behind a pay wall. Accessibility issues can be addressed by having a digital version on websites that are free to users. You can also submit your guidelines to the open access databases mentioned in Section 4.
Provide a number of different ways for people to read or download your guideline. For example, as well as having the guideline available on a website you can upload the summary or full version of guidelines as PDF (portable document format) files.
Consider providing a ‘useful links’ list of hyperlinks on your guideline’s landing page to direct users to relevant sections within your guideline. You can also break up the content into smaller, digestible topics through the use of drop-down menus (Robertson, Smith et al. 2014). The use of infographics or icons instead of plain text can also attract an end user’s interest and improve awareness (Griffon, Kerdelhué et al. 2014; Pereira, Hassler et al. 2014). To ensure broad accessibility, images should use ALT-text, which is a ‘text alternative’ for pictures, allowing a screen reader to read text associated with a screen image (refer to Using alt attributes on img elements).
Using mobile phone applications will enable your guideline to be digitally accessible for many users, although you will need ongoing technical support for the application platforms (Penders and Mallet 2016). Planning and budgeting for application software development or hiring user experience experts to design your website will be an important part of your project plan, including considering any cost impacts.
Be aware of any digital accessibility requirements for end users with special needs such as visual or hearing impairments. Where appropriate you will also need to make sure that your website meets the World Wide Web Consortium’s Web Content Accessibility Guidelines version 2.01 (WCAG 2.1).
The Australian Government Digital Service Standard provides a set of best practice principles for designing and delivering government services including guidelines produced by government agencies. These principles will be useful in developing online versions of your guideline. There are guides and tools available to help make your guideline searchable, navigable and compliant with government accessibility requirements.
7. Implement your strategy
When it is time to release your guidelines, consider an online launch supported by an official launch event, or workshop to help experts, practitioners and related professionals understand your guidelines, for example, the Australian Living guidelines for stroke management, and the Canadian Stroke Best Practice Recommendations 7th Edition. As well as providing promotional exposure for your guideline, this is a good way to acknowledge the work of the guideline development group.
A communication strategy or media management plan should underpin your guideline release. Having a strategy in place will allow for contingencies or risks to be addressed ahead of time with clearly defined responses or approved statements. If you don’t have access to public relations practitioner support, consider hiring media experts or undertake media training to help you with this approach. Keep your organisation’s key leaders and executive appraised of your guideline’s release plans to ensure a united and connected approach when disseminating publicly. This is especially important should any sensitive information need to be carefully managed or be escalated to a leadership level for response.
You may publish the systematic reviews commissioned for the guideline, but to increase awareness of your guideline you can also publish the development process and recommendations in peer-reviewed journals (WHO 2014), for example, the BMJ rapid recommendation series. If you decide to publish in a journal you may need to make decisions regarding authorship and which journals would provide greater accessibility for your target audience.
8. Evaluate effectiveness of dissemination
Dissemination and communication strategies require careful evaluation and feedback from your target audience. This can be gathered using formal methods such as surveys and interviews. Information can also be collected using informal methods such as using an ‘impact log’ to accumulate feedback (WHO 2014).
If you are using social media — Twitter, Facebook, YouTube — it’s possible to track usage and traffic sources using Google Analytics. For example, a Canadian diabetes guideline was evaluated six months after its dissemination. The evaluation study found that the website was viewed a total of 190,291 times by users around the world. The average user also spent up to five minutes on the website (Ke, Casey et al. 2014).
It may be useful to keep a record of where and when you disseminate the guidelines so you can survey changes in awareness and knowledge. This will also make it easier to disseminate any future updates to the guideline’s recommendations.
9. Remember that dissemination is an ongoing process
Dissemination doesn’t just stop once your guideline have been released to your audiences — it extends to future iterations or revised materials. It is your responsibility to disseminate any updates and important to inform people when the guideline is rescinded. Because of these factors it will be critical to set governance procedures in place and ensure that strict version control is adhered to. This will be particularly important as living guidelines become the norm and recommendations are reviewed and updated more frequently.
Useful resources
GIN Dissemination of guidelines
AHRQ (2005) Dissemination planning tool
Australian Government content guide
Writing for NICE: a guide to help you write more clearly
Australian Government digital service standards
Scottish Intercollegiate Guidelines Networks (SIGN) (2015) - A guideline developer's handbook
References
Acknowledgements
NHMRC would like to acknowledge and thank Dr Miyoung Choi (author), Professor Sally Green from Cochrane Australia (editor) and Associate Professor Leena Gupta for their contributions to the development of this module.
Version 5.0. Last updated 6 September 2019.
Suggested citation: NHMRC. Guidelines for Guidelines: Dissemination and communication. https://www.nhmrc.gov.au/guidelinesforguidelines/implement/dissemination-and-communication.
Last updated 6 September 2019.
Appendix 1: Template for planning dissemination
| Domain | Activities | Work plan | ||||
|---|---|---|---|---|---|---|
| Approach | Timeframe | Responsibility | Budget ($) | |||
| Identifying the research | ||||||
| Planning and strategy | ||||||
1. Dissemination Objectives | What is the goal or objective of dissemination? What do you wish to achieve? | e.g. agenda item at face-to-face meeting of guideline development group | By the end of the scoping process (e.g. 1-2 months) | Project manager | ||
2. Target audience (primary, secondary) | Identify your target audience
| |||||
| 3. Key messages | What are the main messages you want to share? | |||||
| 4. Sensitivities |
| |||||
| Selecting channels and materials | ||||||
| 5. Dissemination options | Consider options available to you:
| |||||
| 6. Appropriate materials |
| |||||
| Implementing the strategy | ||||||
| 7. Implementation |
| |||||
| Assessing effectiveness and refining the program | ||||||
| 8. Evaluation plan |
| |||||
| 9. Refining the Dissemination or Communication Strategy |
| |||||