Birthing on Country services offer a culturally safe, holistic approach to the design of maternity services for First Nations peoples and a strategy to improve maternity care outcomes.
The National Health and Medical Research Council (NHMRC)-funded projects led by researchers from Charles Darwin University, The University of Sydney, and Aboriginal and Torres Strait Islander community controlled and mainstream health services have actively applied this approach to developing and evaluating a range of maternity services to deliver improved health outcomes for First Nations mothers, babies and communities.
A landscape format version of this case study is available as a PDF – see Download section below.
Origin
Birthing on Country (BOC) traditionally involved First Nations women giving birth on the land of their ancestors supported by First Nations midwives, ensuring a spiritual connection to the land for the newborn. BOC services are those designed to meet the needs of First Nations families and communities.
Health and wellbeing in the earliest years, beginning with the future mother's wellbeing before she becomes pregnant, enable children to thrive and grow. The provision of integrated, holistic, culturally and clinically safe, effective, appropriate and reliable maternity services is of central importance to ensure that infants are provided with the best start to life.
However, almost half of First Nations mothers live in rural and remote areas,1 many without local midwives or birthing services. These women often experience multiple stressors, such as poverty, food insecurity and overcrowding, and are not able to access culturally safe services as early, or as often, as recommended in pregnancy.
Higher rates of complications in pregnancy (for example, anaemia, infections, diabetes and heart disease) and smoking during pregnancy are common for First Nations mothers1 who are 3 to 5 times more likely to die in childbirth than non-Indigenous Australian women2 and whose babies are almost twice as likely to die in their first year.3
BOC was recommended for First Nations families in the Australian Government's 2010–2015 National Maternity Service Plan and the first national BOC workshop was held in 2012. Researchers working side by side with First Nations partners have spent years building the evidence base to 'make a difference' and prioritise First Nations knowledges and people through culturally and clinically safe maternity services.
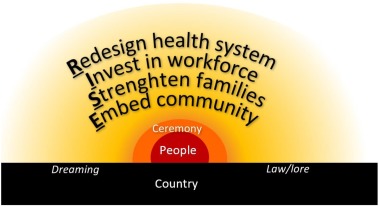
To support scale-up, they have also designed the RISE framework (Redesign the health service, Invest in the workforce, Strengthen families capacity, Embed community control) which respects the knowledge, lore and practices of First Nations communities.
Investment
NHMRC has supported the research described in this case study through:
- a Targeted Call for Research (TCR), 2007: the 1+1 study
- Three Partnership Projects (PSP):
- the Indigenous Birthing in an Urban Setting study (IBUS)
- 2014 Building On Our Strengths (BOOSt)
- 2017 To Be Born Upon a Pandanus Mat, 2021
- A Centre of Research Excellence (CRE), 2020, and multiple Project Grants (PG).
NHMRC has supported the following researchers:
- Professor Sue Kildea: TCR, 2007; PG, 2008 (x2), 2012 (x2), 2016; PSP, 2014, 2015, 2017; CRE, 2020
- Professor Yvette Roe: PSP, 2014, 2017; PG, 2019; TCR, 2020; CRE, 2007, 2020
- Professor Sue Kruske: TCR, 2007; PG, 2012 (x2); PSP, 2014, 2017; CRE, 2020
- Professor Sally Tracy: TCR, 2007; PG, 2008, 2009, 2013; PSP, 2014, 2017
- Emeritus Professor Lesley Barclay: TCR, 2007; PG, 2008, 2009, 2012, 2017; PSP, 2017
- Professor Juanita Sherwood: PG, 2010, 2016, 2018; PSP, 2017; TCR, 2018; CRE, 2020
- Associate Professor Yu Gao: PG, 2012; CRE, 2020
- Professor Roianne West: CRE, 2007, PSP, 2014.
Community engagement
These BOC researchers have spent many years building relationships, developing shared research agendas, fostering deep engagement, and conducting collaborative research with First Nations partner organisations and in First Nations communities. All have worked in multidisciplinary teams side by side with First Nations elders and cultural knowledge holders, Aboriginal Community Controlled Health Services (ACCHS), clinicians, policy advisors and consumers, alongside social scientists, implementation scientists, aeromedical specialists and public health specialists.
Collaborations/ partnerships
The IBUS study, led by Kildea and Roe, was established to monitor, support and improve the implementation of the Birthing in Our Community (BiOC) service, a partnership between the Institute for Urban Indigenous Health (IUIH), the Aboriginal and Torres Strait Islander Community Health Services (ATSICHS), Brisbane, and the Mater Mothers' Hospital.
BOOSt is underway with partner organisations IUIH, Waminda, South Coast Women's Health and Welfare Aboriginal Corporation, ATSICHS, Congress of Aboriginal and Torres Strait Islander Nurses and Midwives, Rhodanthe Lipsett Indigenous Midwifery Charitable Fund and the Australian College of Midwives. It includes researchers from Charles Darwin University (CDU), The University of Queensland, The University of Sydney and Charles Sturt University.
Key components of a BOC service
- Multi-agency partnerships and First Nations governance
- Continuity of midwifery care pre-, during and post-birth
- First Nations workforce
- Cultural Safety framework
- Holistic 'wrap around' services
- Coordinated care integrating primary health network with tertiary services
- Community-based hub, sometimes with a birth centre.

Research
Health services research, undertaken with NHMRC funding, has been used to drive the development, implementation and evaluation of best practice through a number of projects including:
- 1+1=A Healthy Start to Life – Led by Barclay, the study established and evaluated a Midwifery Group Practice to provide continuity of care to First Nations mothers travelling to Darwin for birth, and by designated midwives and child health nurses employed in remote communities in the Northern Territory (NT).
- The Australian Rural Birthing Index (ARBI) – Led by Barclay, the study adapted and evaluated a Canadian tool to guide the provision of maternity services for populations under 25,000 in rural and remote Australia.
- The M@NGO Randomised Clinical Trial of Caseload Midwifery – Led by Tracy and Kildea, the study tested 24/7 caseload Midwifery Group Practice for women regardless of risk factors.
- Evaluating Midwifery Units (EMU) – Led by Tracy, EMU was a prospective cohort study of primary level 2 (free standing) midwifery units across Australia and New Zealand.
- IBUS – Led by Kildea, IBUS evaluated the implementation of the BiOC service in Brisbane, generating high-level evidence of clinical and cultural safety and effectiveness. Early career researcher Dr Sophie Hickey managed IBUS, with community researchers Sarah Maidment and Kayla Heinemann (pictured) recruiting over 600 First Nation families to complete surveys about their pregnancy and postnatal journeys.
- BOOSt – Led by Kildea, this study aims to implement and evaluate a BOC service and facility, including a stand-alone birth centre, in urban (Queensland) and rural areas (New South Wales).
- To Be Born Upon a Pandanus Mat – Led by Roe and commencing in 2021, this project integrates Yolŋu (Assoc. Prof. Lawurrpa Maypilama) and western knowledge (early career researcher Dr Sarah Ireland) systems to support BOC and Yolŋu doulas (djäkamirr).
Health outcomes and impact
- 1+1=A Healthy Start to Life contributed to changed policies and practice for maternal infant health care, improved models of care and changed workforce. The remote Midwifery Group Practice model has been scaled up for all remote communities across the Top End of the NT for women travelling to Darwin for birth.
- ARBI identified that services do not meet need and is being used in at least three states to inform the planning and review of maternity services.
- M@NGO found caseload midwifery care was safe, improved outcomes (for example, reduced elective caesarean sections, increased breastfeeding) and outperformed standard care on every antenatal satisfaction item measured, at reduced cost. Midwifery group practice care is now available for 15% of Australian women.
- EMU found freestanding midwife-led primary-level 2 maternity units to be safe places for women to birth, with higher rates of spontaneous vaginal births and lower rates of interventions and morbidities than for low-risk women who planned a tertiary hospital birth.
- IBUS found an almost 40% reduction in preterm birth, an increase in the First Nations workforce and control over the funding and services. Women were less likely to have an elective caesarean section or epidural in labour, or have their babies admitted to the neonatal unit. Women attended earlier and more often for antenatal care and breastfeeding rates increased. The BiOC service was expanded in 2017 with Queensland Government funding.
- Cultural Safety training (Sherwood and West) is now mandatory for all nurses and midwives wishing to remain registered in 2022 in Australia.
- The BOC CRE will build on different aspects of RISE with 13 projects planned to continue this work.
- To Be Born Upon a Pandanus Mat is underpinned by women's law to incorporate the skills and knowledge of the djäkamirr to enhance the delivery of clinically and culturally safe healthcare.
Timeline
| Year | NHMRC Grant |
|---|---|
| 2007 | TCR (Barclay, Kildea, Kruske, Tracy, Gao) 1+1 study commences in Darwin |
| 2007 | CRE Building Indigenous Research Capacity |
| 2008 | PG (Tracy & Kildea) M@NGO study begins |
| 2008 | PG (Kildea) |
| 2008 | PG (Barclay) |
| 2009 | PG (Tracy & Barclay) EMU study begins |
| 2010 | PG (Sherwood) |
| 2011 | National Maternity Service Plan (2010–2015) |
| 2012 | PG (Kruske) |
| 2012 | PG (Barclay, Kruske & Kildea) ARBI study begins |
| 2012 | PG (Kildea & Gao) |
| 2012 | National BOC Workshop |
| 2013 | PG (Tracy) |
| 2013 | BiOC service established |
| 2014 | Partnership Grant (Kildea, Kruske, Roe, Tracy, & West) IBUS study begins |
| 2014 | PSP (West, Roe) |
| 2016 | Partnership Grant (Kildea) |
| 2016 | PG (Sherwood) |
| 2017 | Partnership Grant (Kildea, Kruske, Tracy, Roe, Barclay, Sherwood) BOOSt begins |
| 2018 | PG & TCR (Sherwood) |
| 2019 | PG (Roe) |
| 2020 | TCR (Roe) |
| 2020 | CRE (Roe, Kildea, Sherwood, Kruske, Gao, Tracy & Barclay) BOC CRE |
| 2021 | Partnership Grant (Roe, Kildea, Gao) Pandanus Mat begins |
Researcher profiles
Prof Sue Kildea
Sue Kildea is a Professor of Midwifery and co-director of the Molly Wardaguga Research Centre at CDU. In 2004, she was a joint recipient of the University of Technology Sydney Human Rights Award. She won Research Australia's Health Services Research Award in 2018.
Prof Yvette Roe
Yvette Roe is a Professor of Indigenous Health and co-director of the Molly Wardaguga Research Centre at CDU. She is a Njikena Jawuru woman from the West Kimberley region of Western Australia with more than 25 years' experience working in the Indigenous health sector.
Prof Sue Kruske
Sue Kruske is Professor in Primary Health Care at CDU's College of Nursing and Midwifery. She is a midwife and child health nurse and was the Regional Manager of Maternal Child Health at IUIH from 2014–19 and oversaw the BiOC service.
Prof Juanita Sherwood
Juanita Sherwood is Professor of Decolonisation in Health, Education and Research at the CDU Molly Wardaguga Research Centre and works closely with Grandmothers against removals. She is a nurse, teacher, lecturer and researcher in First Nations health and education and a board member and Elder of the Congress of Aboriginal and Torres Strait Islander Nurses and Midwives (CATSINaM) Elders Circle.
Prof Roianne West
Roianne West is a Professor of Workforce Innovation at the Molly Wardaguga Research Centre at CDU and CEO of CATSINam. She is a Kalkadunga and Djaku-nde woman who began her work in Aboriginal health research and health workforce reform 25 years ago at an ACCHS.
A/Prof Yu Gao
Yu Gao is an Associate Professor and Research Focussed Principal Fellow at the Molly Wardaguga Research Centre at CDU. An obstetrician, she also has extensive experience in medical biostatistics, social science and health economic research.
Prof Sally Tracy
Sally Tracy is Emeritus Professor of Midwifery at The University of Sydney and is an expert in maternity services research, costing analysis, randomised trials and cohort studies in New Zealand and Australia. She led the NHMRC M@NGO trial, laying the foundation for the BiOC service.
Prof Lesley Barclay AO
Lesley Barclay is Emeritus Professor at the University Centre for Rural Health, School of Public Health, The University of Sydney. She is an educational leader, health services researcher and systems reformer and was made an Officer of the Order of Australia in 2004.
RISE
Projects described in this case study led to the development of the RISE Translation Framework, underpinned by a worldview of Indigenous relationality (interconnectedness), 'Country', people (at the centre), dreaming (creation), law/lore (cultural practices, customs, laws and protocols) and ceremony.4 RISE has been translated into Yolŋu Matha language by Associate Professor Lawurrpa Maypilama, a senior cultural knowledge holder, and Dr Sarah Ireland and is being used to redesign services in north-east Arnhem Land – the 'very remote BOC demonstration site'.5 RISE is intended to provide a robust framework to guide future research and translation.
References
This case study was developed in partnership with the lead researchers named in this work.
The information and images from which NHMRC Impact Case Studies are produced may be obtained from a number of sources including our case study partner, NHMRC's internal records and publicly available materials.
- Australian Institute of Health and Welfare. Pregnancy and birth outcomes for Aboriginal and Torres Strait Islander women 2016–2018. Cat. no. IHW 234. Canberra: AIHW; 2021
- Australian Institute of Health and Welfare. Maternal deaths in Australia. Canberra: AIHW; 2020
- Australian Institute of Health and Welfare 2021. Pregnancy and birth outcomes for Aboriginal and Torres Strait Islander women 2016–2018. Cat. no. IHW 234. Canberra: AIHW; 2021
- Kildea S, Hickey S, Barclay L, Kruske S, Nelson C, Sherwood J, Allen J, Gao Y, Blackman R, Roe YL. Implementing birthing on country services for Aboriginal and Torres Strait Islander families: RISE framework. Women and Birth. 2019;32(5):466–75
- Ireland S, Maypilama EL, Roe Y, Lowell A, Kildea S. Caring for Mum On Country: Exploring the transferability of the Birthing On Country RISE framework in a remote multilingual Northern Australian context. Women and Birth. 2021;34(5):487–92
Further information
Further information about BOC and the studies mentioned in this case study can be found in the references below:
Allen J, Kildea S, Hartz DL, Tracy M, Tracy S. The motivation and capacity to go 'above and beyond': Qualitative analysis of free-text survey responses in the M@NGO randomised controlled trial of caseload midwifery. Midwifery 2017;50:148–56
Allen J, Kildea S, Stapleton H. How does group antenatal care function within a caseload midwifery model? A critical ethnographic analysis. Midwifery 2015;31:489–97
Barclay L, Kornelsen J, Longman J, Robin S, Kruske S, Kildea S, Pilcher J, Martin T, Grzybowski S, Donoghue D, Rolfe M. Reconceptualising risk: Perceptions of risk in rural and remote maternity service planning. Midwifery. 2016;38:63–70
Barclay L, Kruske S, Bar-Zeev S, Steenkamp M, Josif C, Narjic CW, Wardaguga M, Belton S, Gao Y, Dunbar T, Kildea S. Improving Aboriginal maternal and infant health services in the 'Top End'of Australia; synthesis of the findings of a health services research program aimed at engaging stakeholders, developing research capacity and embedding change. BMC Health Services Research. 2014;14(1):1–9
Gao Y, Gold L, Josif C, Bar-Zeev S, Steenkamp M, Barclay L, Zhao Y, Tracy S, Kildea S. A cost-consequences analysis of a Midwifery Group Practice for Aboriginal mothers and infants in the Top End of the Northern Territory, Australia. Midwifery. 2014;30(4):447–55
Hickey S, Couchman K, Stapleton H, Roe Y, Kildea S. Experiences of health service providers establishing an Aboriginal-Mainstream partnership to improve maternity care for Aboriginal and Torres Strait Islander families in an urban setting. Evaluation and Program Planning. 2019;77:101705
Hickey S, Kildea S, Couchman K, Watego-Ivory K, West R, Kruske S, Blackman R, Watego S, Roe YL. Establishing teams aiming to provide culturally safe maternity care for Indigenous families. Women and Birth. 2019;32(5):449–59
Hickey S, Roe Y, Gao Y, Nelson C, Carson A, Currie J, Reynolds M, Wilson K, Kruske S, Blackman R, Passey M. The Indigenous Birthing in an Urban Setting study: the IBUS study. BMC Pregnancy and Childbirth. 2018;18(1):1–2
Hickey SD, Maidment S-J, Heinemann KM, Roe YL, Kildea SV. Participatory action research opens doors: Mentoring Indigenous researchers to improve midwifery in urban Australia. Women and Birth. 2018;31:263–8
Josif C, Barclay L, Bar-Zeev S, Kildea S, Brittin M. How participatory action research supported improvements to the postnatal discharge summary system used for remote dwelling Aboriginal mothers and infants in the Top End of Australia. Action Research. 2012;10:387–405
Kelly, J, West R, Gamble J, Sidebotham M, Carson V and Duffy E. 'She knows how we feel': Australian Aboriginal and Torres Strait Islander childbearing women's experience of Continuity of Care with an Australian Aboriginal and Torres Strait Islander midwifery student. Women and Birth. 2014;27(3):157–162
Kildea S, Barclay L, Wardaguga M, Dawumal M. Participative research in a remote Australian Aboriginal setting. Action Research. 2009;7:143–63
Kildea S, Gao Y, Hickey S, Kruske S, Nelson C, Blackman R, Tracy S, Hurst C, Williamson D, Roe Y. Reducing preterm birth amongst Aboriginal and Torres Strait Islander babies: a prospective cohort study, Brisbane, Australia. EClinicalMedicine. 2019;12:43–51
Kildea S, Gao Y, Hickey S, Nelson C, Kruske S, Carson A, Currie J, Reynolds M, Wilson K, Watego K, Costello J. Effect of a Birthing on Country service redesign on maternal and neonatal health outcomes for First Nations Australians: a prospective, non-randomised, interventional trial. The Lancet Global Health. 2021;9(5):e651–9
Kildea S, Gao Y, Rolfe M, et al. Remote links: Redesigning maternity care for Aboriginal women from remote communities in Northern Australia – A comparative cohort study. Midwifery 2016;34:47–57
Kildea S, Hickey S, Nelson C, Currie J, Carson A, Reynolds M, Wilson K, Kruske S, Passey M, Roe Y, West R. Birthing on Country (in Our Community): a case study of engaging stakeholders and developing a best-practice Indigenous maternity service in an urban setting. Australian Health Review. 2017;42(2):230–8
Kildea S, Lockey R, Roberts J and Magick-Dennis F (2016). Guiding principles for developing a Birthing on Country service model and evaluation framework, Phase 1. Brisbane, Mater Medical Research Unit and the University of Queensland, on behalf of the Maternity Services Inter-Jurisdictional Committee for the Australian Health Ministers' Advisory Council
Kildea, S, Magick, DF, Stapleton H (2012). Birthing on country: workshop report. Brisbane, Australia: Maternity Services Inter-Jurisdictional Committee
Kildea S, Van Wagner V. 'Birthing on Country,' Maternity Service Delivery Models: A review of the literature. Canberra (ACT), Maternity Services Inter-Jurisdictional Committee for the Australian Health Minister's Advisory Council; 2018. Available from: https://www.saxinstitute.org.au/wp-content/uploads/Birthing-on-Country1.pdf
Kruske S, Belton S, Wardaguga M, Narjic C. Growing up our way: the first year of life in remote Aboriginal Australia. Qualitative Health Research. 2012;22(6):777–87
Kruske S, Schultz T, Eales S, Kildea S. A retrospective, descriptive study of maternal and neonatal transfers, and clinical outcomes of a Primary Maternity Unit in rural Queensland, 2009–2011. Women and Birth. 2015;28(1):30–9
Kruske, S. Characteristics of culturally competent maternity care for Aboriginal and Torres Strait Islander women. Maternity Services Inter-jurisdictional Committee for the Australian Health Ministers Advisory Council; 2011
Lowell A, Kildea S, Liddle M, Cox B, Paterson B. Supporting Aboriginal knowledge and practice in health care: lessons from a qualitative evaluation of the strong women, strong babies, strong culture program. BMC Pregnancy and Childbirth 2015;15:19
Lowell A, Maypilama EL, Fasoli L, Gundjarranbuy R, Godwin-Thompson J, Guyula A, Yunupiŋu M, Armstrong E, Garrutju J, McEldowney R. Building Yolŋu skills, knowledge, and priorities into early childhood assessment and support: protocol for a qualitative study. JMIR Research Protocols. 2018;7(3):e8722
Lowell A, Maypilama Ḻ, Fasoli L, Guyula Y, Guyula A, Yunupiŋu M, Godwin-Thompson J, Gundjarranbuy R, Armstrong E, Garrutju J, McEldowney R. The 'invisible homeless' – challenges faced by families bringing up their children in a remote Australian Aboriginal community. BMC Public Health. 2018;18(1):1–4
Monk A, Tracy M, Foureur M, Grigg C, Tracy S. Evaluating Midwifery Units (EMU): a prospective cohort study of freestanding midwifery units in New South Wales, Australia. BMJ open. 2014;4(10):e006252
Monk A, Tracy M, Foureur M, Barclay L. Australian primary maternity units: Past, present and future. Women and Birth. 2013;26(3): 216–218
Roe Y, Briggs M, Buzzcott C, Sherwood J, Kildea S. Returning birthing services to communities and Aboriginal control: Aboriginal women of Shoalhaven Illawarra Region describe how Birthing on Country is linked to healing. Journal of Indigenous Wellbeing. 2020;5(1):58–71
Sherwood J, Kendall S. Reframing spaces by building relationships: Community collaborative participatory action research with Aboriginal mothers in prison. Contemporary Nurse. 2013;46:83–94
Tracy SK, Hartz DL, Tracy MB, et al. Caseload midwifery care versus standard maternity care for women of any risk: M@NGO, a randomised controlled trial. The Lancet. 2013;382:1723–32
Tracy SK, Dahlen H, Caplice S, Laws P, Wang YA, Tracy MB, Sullivan E. Birth Centers in Australia: A National Population-Based Study of Perinatal Mortality Associated with Giving Birth in a Birth Center. Birth. 2007;34(3):194–201
West, R, Armao JE, Creedy DK, Saunders V and Rowe Minnis F. Measuring effectiveness of cultural safety education in First Peoples health in university and health service settings. Contemporary Nurse. 2021;57(5):356–369
West R, Gamble J, Kelly J, Milne T, Duffy E and Sidebotham M. Culturally capable and culturally safe: Caseload care for Indigenous women by Indigenous midwifery students. Women and Birth. 2016;29(6):524–530
West R, Mills K, Rowland D and Creedy DK. Validation of the first peoples cultural capability measurement tool with undergraduate health students: A descriptive cohort study. Nurse Education Today. 2018;64:166–171
West R, Wrigley S, Mills K, Taylor K, Rowland D and Creedy DK. Development of a First Peoples-led cultural capability measurement tool: A pilot study with midwifery students. Women and Birth. 2017;30(3):236–244.
Birthing on Country
The term 'Birthing on Country' was defined by the Australian Government Maternity Services Interjurisdictional Committee as:
Maternity services designed and delivered for Indigenous women that encompass some or all of the following elements: are community based and governed; allow for incorporation of traditional practice; involve a connection with land and country; incorporate a holistic definition of health; value Indigenous and non-Indigenous ways of knowing and learning; risk assessment and service delivery; are culturally competent; and developed by, or with, Indigenous people.
At the Birthing on Country workshop (July 2012, Alice Springs), an Aboriginal elder, Djapirri Mununggirritj, a Yolngu woman from north-east Arnhem Land in the Northern Territory, further described it as:
Birthing on Country should be understood as a metaphor for the best start in life for Aboriginal and Torres Strait Islander babies and their families because it provides an integrated, holistic and culturally appropriate model of care; not only bio-physical outcomes … it's much, much broader than just the labour and delivery … (it) deals with socio-cultural and spiritual risk that is not dealt with in the current systems. It is important that the Birthing on Country project move from being aspirational to actual. The Birthing on Country agenda relates to system-wide reform and is perceived as an important opportunity in 'closing the gap' between Indigenous and non-Indigenous health and quality of life outcomes.