Infants are vulnerable to health challenges because of the relatively immature state of their bodies, including their nervous, cardiovascular and respiratory systems. Moreover, an infant may appear completely healthy but still have an underlying vulnerability that can make it difficult for that infant to cope with certain kinds of environmental stress.
NHMRC-funded researchers at the Menzies Institute for Medical Research, at the University of Tasmania, made a major contribution to protecting infants by providing compelling evidence for the existence of one such stressor – ‘on tummy’ sleeping.
A landscape format version of this case study is available as a PDF from the Downloads section below.
Origin
The sudden death of infants from unknown causes (also known as ‘cot death’) was brought to NHMRC’s attention as early as 1951. A report from the Walter and Eliza Hall Institute noted that many deaths of this type had been reported as due to accidental suffocation and that the Institute was investigating the possibility of other causes.1
In 1970, Dr Susan Beal, from the Department of Pathology at the Adelaide Children’s Hospital, was asked to investigate the incidence of Sudden Infant Death Syndrome (SIDS) in South Australia.2 In 1972, she reported that SIDS was responsible for the deaths of more children between 2 weeks and 2 years of age (about 30-35 per year) than any other single condition.3 In fact, SIDS had become the commonest cause of death in postneonatal infants in Australia.4
Beal observed that SIDS 'too often results in not only the tragedy of the death, but for the parents unwarranted self-recrimination and external blame, and therefore much needless suffering. The condition should be explained to parents and understood by the community.' 3

Grants and Investment
In 1985, when Dr Terry Dwyer moved to the University of Tasmania to establish an epidemiology research centre (now known as the Menzies Institute for Medical Research), the annual rate of SIDS in Tasmania was twice the national average.5
Despite the gradual accumulation of retrospective (after death) evidence of an association between prone (on tummy) sleeping and SIDS, the medical community had not accepted sleeping position as a cause.4 There had, in fact, been an increase in the prevalence of prone sleeping among healthy infants in many Western countries from the late 1960s and 1970s into the 1980s, due to the provision of non-scientifically tested advice to parents.6 Data that excluded recall bias (by being obtained before SIDS had occurred) and that measured potentially important confounders were needed to make a compelling case against prone sleeping.7
To address this gap, the Menzies team commenced the Tasmanian Infant Health Survey (TIHS). The research program was led by Terry Dwyer. Anne-Louise Ponsonby, an early career doctor, assumed responsibility for coordinating both the birth cohort and a concurrent death scene case control study as part of her NHMRC-funded PhD thesis on SIDS, supervised by Dwyer. Laura Gibbons provided biostatistical expertise and Neville Newman, a paediatrician and neonatologist, contributed key clinical and scientific insights. The TIHS research was supported by five NHMRC grants.
Other funding
TIHS was supported by the: Australian Rotary Health Research Fund, US National Institutes of Health, Tasmanian State Government, National SIDS Council of Australia, Sudden Infant Death Research Foundation of Victoria, Australian Government Department of Health, Zonta International, Wyeth Pharmaceuticals, Tasmanian Sanatoria After-Care Association and other organisations.8
Research
TIHS was a prospective cohort study, which meant that it followed, over time, a group of similar individuals (cohorts) who differed with respect to certain factors under study (e.g. sleeping position) to determine how these factors affected rates of a certain outcome (i.e. SIDS).
The first full TIHS data collection commenced in 1988 and was a huge endeavour. The six obstetric hospitals taking part in the survey covered approximately 93% of live births in Tasmania.
From January 1988 to March 1990, 3,110 infants were eligible for the survey, which involved interviews with mothers, a developmental assessment of the infant and taking measurements of the infant and its sleeping environment. For each infant, these activities took place on three occasions during its first three months after birth.
In May 1991, the team at Menzies published the first results of the study, the first of its kind in the world. Their findings supported the view that prone sleeping should not be advocated for infants unless there were specific clinical indications to do so.7
In 1993, the team published further findings showing that the adverse risk of the prone position was significantly increased by several factors including the type of mattress used, swaddling, recent illness and heating of the infant’s room.9
By 1995, when the survey ended, the cohort numbered 11,000 infants and children5 and the survey had collected longitudinal data on approximately one in five live births in Tasmania. Using these data, the Menzies team provided further compelling evidence that prone sleeping was a significant risk factor for SIDS and that sleep position changes were responsible for the majority of the decline in the SIDS rate.10
Results and Translation
The published findings of the Menzies’ team’s research led to a rapid policy response. Beginning in May 1991, the team ensured that, after usual sleeping position data had been collected, every participant in the cohort had been informed of the study finding that prone-sleeping infants were at increased risk of SIDS.10
In June 1991, the ‘Reducing the Risks of Cot Death’ health education campaign was formally launched by the National SIDS Council of Australia.11 In July 1991, a national meeting provided a new recommendation that healthy infants should not sleep prone. SIDS Australia incorporated the finding into health education advice to new parents.4 In October 1991, NHMRC released a statement on SIDS, drafted by its Child Health Committee.12
NHMRC’s 1991 statement on SIDS (excerpt)
Council notes recent reports regarding risk factors for Sudden Infant Death Syndrome (SIDS). The possible causes of SIDS are still not known. However, population studies have identified risk factors that may contribute to SIDS. Risk factors that parents may be able to do something about include sleeping posture, feeding practices and passive smoking.
Recent research studies suggest that babies who sleep on their stomach may have a higher risk of SIDS. It is recommended that babies should generally sleep on their side or on their back. If on their side, the lower arm should be placed well forward so that babies cannot roll on their stomach.
A similar recommendation was issued by the American Academy of Pediatrics in the United States in 1992.13 Dwyer and Ponsonby contributed to the development of such recommendations both in Australia and overseas.
Health Outcomes and Impact
The death rate from SIDS fell so rapidly after the prone sleeping position campaign that, by late 1991, it was clear there would eventually be insufficient cases occurring annually in Tasmania for data collection in the survey. When Menzies started its research there had been an average of 27 cases a year for an extended period but by 1998 there were only three.5
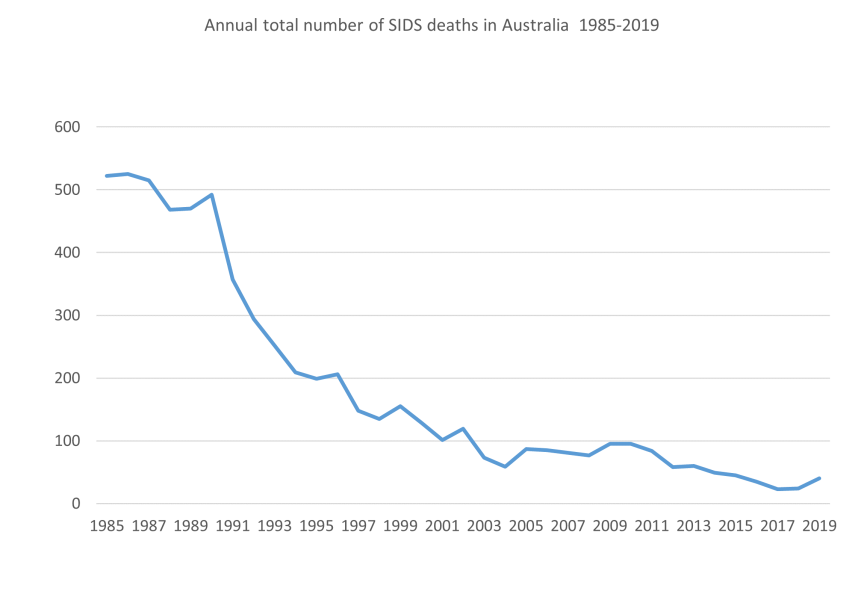
In Australia as a whole the number of SIDS deaths declined from 522 in 1985 to 73 in 2003, a reduction of 86%.20 Significant reductions occurred in other countries where campaigns to change sleeping position had occurred.15
Since its inception, the ‘safe sleeping intervention’ may have saved more than 7,000 infant lives per year. As most of these infants were otherwise healthy and were born in higher income countries where life expectancy is of the order of 80 years, it can be estimated that >500,000 years of life have been gained per year from the intervention. The number could be considerably higher as accurate data on lives saved are not available for large parts of the world.16
Timeline
| Date | Event |
|---|---|
| 1985 | Dwyer commences at University of Tasmania |
| 1988 | SIDS cases in Tasmania average 27 per year Tasmanian Infant Health Survey (TIHS)(1988-1995) |
| 1989 | Postgraduate Scholarship (Ponsonby) |
| 1990 | Project Grant (Dwyer) |
| 1991 | Project Grant (Dwyer) National SIDS campaign launched NHMRC statement on SIDS |
| 1992 | Targeted Call for Research (Dwyer, Newman, Ponsonby) |
| 1994 | Early Career Fellowship (Ponsonby) |
| 1998 | SIDS cases in Tasmania reduced to 3 per year |
Researcher profiles
Dr Susan M Beal AM
Susan Beal studied medicine at The University of Sydney and specialised in paediatrics. During the 1960s she worked at the Adelaide Children's Hospital as a research registrar in neurosurgery and then ran the Cerebral Palsy Clinic. Beal pioneered SIDS research and, between 1973 and 1990, visited more than 500 families in South Australia who had lost babies to SIDS. She gathered information from the scene in which the baby died and from the bereaved families. Beal was appointed a Member of the Order of Australia in 1997, for service to medicine, particularly in the fields of paediatrics and SIDS research.
Professor Terry Dwyer AO
Terry (Terence) Dwyer worked at CSIRO and the Commonwealth Institute of Heath at The University of Sydney before moving to the University of Tasmania. He was Director of the Menzies Institute (1988-2003), Director of the Murdoch Children’s Research Institute (MCRI) (2004-2014) and Executive Director of The George Institute for Global Health at the University of Oxford (2014-2018). Dwyer was awarded the Australian Society for Medical Research Medal in 2003 and was made an Officer of the Order of Australia in 2005 in recognition of his SIDS research and contributions to medical research.
Professor Anne-Louise Ponsonby
Anne-Louise Ponsonby has worked in various roles including as the Foundation Chair of Population Health at The Australian National University Medical School. Ponsonby is now an epidemiologist and public health physician based at The Florey Institute of Neuroscience and Mental Health in Melbourne. She has extensive experience in the design, conduct and analysis of population-based studies. Her current work is focused on combining population epidemiologic approaches with system biology, and using this approach, within population-based studies, to investigate early brain development and multiple sclerosis.
Dr Neville M Newman
Neville Maurice Newman (1923-2018) was a consultant paediatrician and Director of Neonatology at the Royal Hobart Hospital. He was a Doctor of Surgery, a Fellow of the Royal Australasian College of Physicians and a Fellow of the Royal College of Physicians (London).
Dr Laura E Gibbons
Laura Gibbons is a General Internal Medicine Biostatistician at the University of Washington and a Data Management and Statistics Core researcher at the University of Pittsburgh Alzheimer’s Disease Research Center.
Sudden Infant Death Syndrome (SIDS)
The term ‘SIDS’ is used when an infant, who has apparently been quite well, is found unexpectedly dead and follow-up examination is unable to discern a cause of death.
SIDS is thought to occur when a vulnerable infant is exposed to environmental stressors.
Infants are particularly vulnerable between two to four months following birth, as during this time the infant brain is undergoing rapid and extensive physiological changes, particularly in how it controls activities such as breathing and the maintenance of body temperature.
Infants may be particularly vulnerable during sleep because of dysfunctional and/or immature cardio-respiratory and/or arousal systems that make it difficult for them to respond to stressors.
External environmental stressors include prone (on tummy) sleeping, overheating with excessive bedding, co-sleeping and soft bedding. Epidemiological studies on the incidence of SIDS have also identified that maternal smoking or drug addiction may enhance the vulnerability of a developing infant. Conversely, there are external factors that may be protective against SIDS, such as breastfeeding.23, 24
References
This case study was developed with input from Professor Anne-Louise Ponsonby and Professor Terry Dwyer, and in partnership with the Menzies Institute for Medical Research at the University of Tasmania.
The information and images from which impact case studies are produced may be obtained from a number of sources including our case study partner, NHMRC’s internal records and publicly available materials.
The following sources were consulted for this case study:
1 National Health and Medical Research Council. Report of the National Health and Medical Research Council, Thirty–first session held at Sydney NSW, 23rd and 24th May 1951. NHMRC. p190
2 Australian Women’s Archives Project. The Australian women’s register: Beal, Susan (1935- ). Available from: http://www.womenaustralia.info/biogs/AWE0951b.htm. 2004. Accessed 20 September 2021
3 Beal S. Sudden Infant Death Syndrome. MJA 1972; 2: 1223–1229. [Quote taken from p1228]
4 Van Der Weyden MB. Bench-to-bedside research in Australian research institutes – a snapshot. MJA 2003; 179(11): 603-610
5 Dwyer T. The Research Enterprise - The Menzies Centre for Population Health Research. MJA 2001; 175(11): 617–620
6 Hogberg U, Bergstrom E: Suffocated prone: the iatrogenic tragedy of SIDS. Am J Public Health 2000; 90: 527-531
7 Dwyer T, Ponsonby AL, Newman NM, Gibbons LE. Prospective cohort study of prone sleeping position and sudden infant death syndrome. Lancet 1991; 337: 1244–1247
8 Ponsonby AL, Couper D, Dwyer T, Carmichael A, Kemp A, Cochrane J. The Relation between Infant Indoor Environment and Subsequent Asthma. Epidemiology 2000; 11(2): 128–135
9 Ponsonby AL, Dwyer T, Gibbons LE et al. Factors potentiating the risk of SIDS associated with the prone position. N Engl J Medicine 1993; 329: 377–382
10 Dwyer T, Ponsonby AL, Blizzard CL et al. The contribution of changes in the prevalence of prone sleeping position to the decline in SIDS in Tasmania. JAMA 1995; 273: 783–789
11 Raven L. Sudden Infant Death Syndrome History. Chapter 4 in in SIDS - Sudden infant and early childhood death: The past, the present and the future. Duncan JR, Byard RW (eds). 2018. The University of Adelaide Press
12 National Health and Medical Research Council. Report of the National Health and Medical Research Council, 112th session October 1991. NHMRC. p46
13 American Academy of Pediatrics (AAP) Task Force on Infant Positioning and SIDS: Positioning and SIDS. Pediatrics 1992; 89(6): 1120–1126
14 Australian Institute of Health and Welfare. General Record of Incidence of Mortality (GRIM) books. AIHW. Accessed from https://www.aihw.gov.au/reports/life-expectancy-deaths/grim-books/contents/grim-excel-workbooks. Version 25 June 2021
15 Sidebotham S, Bates F, Ellis C, Lyus L. Preventive Strategies for Sudden Infant Death Syndrome. Chapter 12 in SIDS - Sudden infant and early childhood death: The past, the present and the future. Duncan JR, Byard RW (eds). 2018. The University of Adelaide Press
16 Personal communication, Professor Terry Dwyer, 25 October 2021
17 Duncan JR, Byard RW. Sudden Infant Death Syndrome: An Overview. Chapter 2 in SIDS - Sudden infant and early childhood death: The past, the present and the future. Duncan JR, Byard RW (eds). 2018. The University of Adelaide Press
18 Gaultier C. Environmental Factors and Risk for SIDS. Pediatr Res 1999; 45: 36.
Partners
