Until the 1970s, people experiencing infertility had few options. Commencing in the late 1960s, NHMRC-funded researchers at Monash University and other research centres in Melbourne began creating in vitro fertilisation (IVF) technologies and developed them into robust medical procedures that are now used worldwide. These technologies have significantly expanded the options available for those wishing to have a baby and today IVF is responsible for about 1 in 20 births in Australia.
A landscape format version of this case study is available as a PDF from the Downloads section below.
Origin
As early as 1937, NHMRC received reports referring to the phenomenon of ‘sterility’: infertility that led to childlessness in married couples. In 1944, NHMRC established a Committee of Inquiry into the Medical Aspects of the Decline in the Birth-rate that was intended to “investigate the incidence . . . of primary sterility in both females and males”, to report on its causes and to make recommendations on how it might be prevented or cured.
By 1945, NHMRC was providing financial assistance to nine fertility clinics across Australia that were working to understand the incidence and impacts of infertility.
During the late 1960s and early 1970s, about one in ten Australian women of reproductive age experienced infertility, with half of these women seeking some form of treatment.1 At this time, treatment for infertile women and men was limited and, due to the introduction of the oral contraceptive pill in 1961, fewer babies from unplanned pregnancies were being placed for adoption.2
In vitro fertilisation (IVF) technologies had been used successfully in non-human mammals since 1959.3 These technologies enabled an egg to be fertilised with a sperm in a laboratory setting and the resultant fertilised embryo to be transplanted into the uterus with the intention of forming a successful pregnancy.
Internationally, medical researchers began looking to IVF as a potential treatment, primarily for tubal factor infertility (blocked fallopian tubes) in women.
Infertility affects about 1 in 6 Australian couples of reproductive age and affects men and women equally often. Its causes are varied and include: problems with the production of sperm or eggs; the structure or function of male or female reproductive systems; and/or hormonal and immune conditions.4
Grants and Investment
NHMRC began funding IVF-related research during the late 1960s, at a time when IVF techniques were first being developed.
Over the following three decades, NHMRC supported the development of human IVF technologies through a succession of grants to researchers who were predominantly based at Monash University.
These researchers were:
- Carl Wood (funded 1966-74)
- John Leeton (1967-72)
- Alan Trounson (1977-2000) – also supported by a grant from the Ford Foundation and US National Institutes of Health (NIH) grants.
- Henry Sathananthan (1986-94)
- Ismail Kola (1986-98)
- Dougal Macfarlane (1987-91)
- Jillian Shaw (1991-2000).
NHMRC also provided support to Alex Lopata (1971-95), based at the University of Melbourne (UoM), Royal Women’s Hospital (RWH) and Queen Victoria Hospital (QVH).
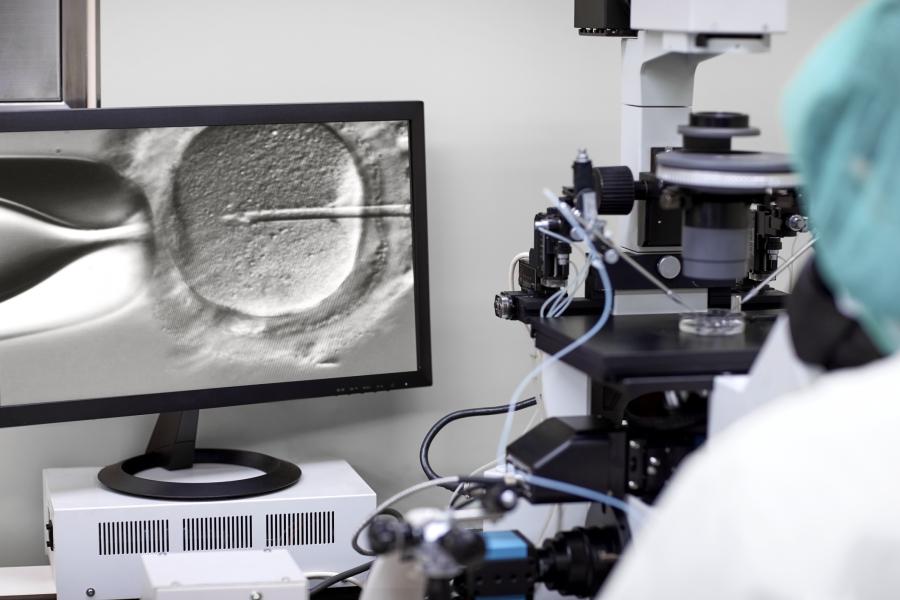
Research and Collaborations
Early studies led by Wood set about transforming IVF into a replicable clinical treatment for infertility.
From 1969-1972, Wood and his team investigated the effects of pharmaceutical and hormonal stimulation of the human ovary. Using hormones to stimulate the ovulation cycle, they discovered how to control egg maturation and egg collection.
In 1970, Wood, Leeton and Lopata formed a collaborative IVF research program known as the ‘Melbourne Egg Project’ (MEP). They were joined by Ian Johnston in 1975 and Trounson in 1977. By 1973, Leeton produced the world’s first human IVF pregnancy. The pregnancy lasted nine days following implantation, ending in early miscarriage.
In 1980, the MEP team was responsible for the birth of Australia’s first IVF baby (and third in the world), Candice Reed, at RWH. Following her birth, the MEP team disbanded and Trounson, Wood and Leeton went on to lead IVF research at Monash University. Wood became the first Head of the Department of Obstetrics and Gynaecology at Monash University.
The team led research that incorporated superovulation (the use of drugs to stimulate the ovary) and control of ovulation to collect multiple mature eggs within a cycle. Other research involved improving culture media, embryo transfer and laparoscopic egg pick-up.
Rather than waiting for natural cycles, these researchers now had precise control over the timing of recovery of the immature ova (egg cells), enabling IVF to be conducted at practical times within clinical environments.
From 1981 to 1991, much of this team’s research focused on cryopreservation and vitrification – techniques for freezing of eggs and embryos. The development of these techniques was informed by Sathananthan’s research and electron microscopic observations of the ultrastructure of human eggs and embryos.
Results and Translation
Trounson and his team’s research on cryopreservation led to the development of robust freezing techniques that allowed embryos, in particular, to be preserved and later thawed for use in IVF cycles.
By 1985, these techniques had been adopted by IVF clinics across Australia. Cryopreservation allowed transfer of a single embryo to the uterus, reducing the serious risks associated with multiple pregnancies.
Other notable developments included:
- the first multiple pregnancies of twins (1981), triplets (1982) and quadruplets (1984)
- the first IVF birth from donor eggs (1983)
- the first IVF birth from a frozen embryo (1984)
- facilitating pregnancies using surgically removed sperm (from 1985)
- sperm microinjection into oocytes to address male infertility (1987-1992)
- the first IVF pregnancies delivered by a surrogate (1988)
- development of embryo biopsy for inheritable genetic disease (1989)
- discovery of human embryonic stem cells (2000).
Recognising the significant advances in IVF technologies and in response to sector feedback, in 1981 NHMRC formed a working party to revise the existing Statement on Human Experimentation. At this time, there were no clear guidelines to assist bioethics committees and research institutions in covering matters associated with IVF.
The working party considered the moral, ethical and scientific concerns raised by IVF and was tasked with formulating guidelines for institutional ethics committees. These guidelines were published in 1982, becoming the first national ethical guidelines on IVF in the world.
Health Outcomes and Impact
Australian researchers pioneered advances that expanded the use of IVF technology. What was originally developed as a treatment for women with blocked fallopian tubes is now being used to overcome a range of fertility issues including obstetric and gynaecological conditions, genetic disorders, age-related infertility and unexplained infertility.
The number of babies born through IVF has steadily increased since the first IVF birth in 1978. In Australia, the number of births as the result of IVF treatment rose from 2,237 (or 0.9% of all births) in 1992 to 4,801 (or 1.9%) in 2000. By 2018, there were 14,355 babies born through IVF, representing almost 1 in 20 babies (or 5%).5
IVF has helped to lessen the impacts of infertility and has enabled many people to conceive, carry and/or deliver children of their own who would have otherwise been unable to.
There is an ever-increasing demand for fertility treatment and research is ongoing to optimise IVF success rates. Modern IVF methods continue to be founded on many of the discoveries of NHMRC-funded researchers.
Monash University interests in the spinout company Monash IVF were sold in 2007 and Monash IVF Group is now listed on the Australian stock exchange.
The current (2017) Ethical guidelines on the use of assisted reproductive technology in clinical practice and research are the latest in a series of revisions to the original 1982 guidelines.
Timeline
| Date | Event |
|---|---|
| 1968 | Grants (Wood) |
| 1969 | Grant (Wood) |
| 1970 | Grant (Wood) |
| 1971 | Grants (Wood, Lopata) |
| 1972 | Grants (Wood, Lopata, Leeton) |
| 1973 | Grants (Wood) |
| 1974 | Grants (Wood) |
| 1975 | Grants (Lopata) Ford Foundation Grant (1975-79) |
| 1978 | Project Grants (Trounson, Lopata) |
| 1979 | Grant (Lopata) |
| 1980 | First IVF birth in Australia Project Grants (Trounson, Leeton) |
| 1981 | IVF working party formed Project Grants (Trounson, Leeton) |
| 1982 | Project Grants (Leeton, Lopata) |
| 1983 | Project Grants (Lopata) Guidelines published |
| 1984 | First birth from a frozen embryo Project Grants (Trounson, Lopata) |
| 1985 | Project Grants (Lopata) |
| 1986 | Project Grants (Trounson, Kola) Infrastructure Grant (Trounson) |
| 1987 | Project Grants (Trounson, Lopata) |
| 1988 | Project Grants (Trounson, Lopata) |
| 1989 | Project Grant (Trounson) Infrastructure Grant (Trounson) |
| 1990 | Project Grants (Trounson) |
| 1991 | Project Grant (Shaw) |
Researcher profiles
Prof Carl Wood CBE AC
Carl Wood (1929-2011) was an Australian gynaecologist and chairman of the Department of Obstetrics and Gynaecology at Monash University (1964-1992). Wood led the Monash IVF team throughout the pioneering developments of IVF technologies in the 1970s and 1980s and was a member of NHMRC’s Maternal Health and Reproduction (Standing) Committee. Later, he was medical director of Monash IVF (1994-2002) and ran a private practice in Melbourne. He was made a Commander of the British Empire in 1981 and a Companion of the Order of Australia in 1995.
Prof Alan Trounson AO
Alan Trounson commenced work at Monash University in 1977. He was appointed Director of the Centre for Early Human Development at Monash University in 1986 and then Deputy Director of the Monash Institute for Reproduction and Development (1990-2003). In 2004, he founded the Monash Immunology and Stem Cell Laboratories and from 2007-2014, he was President of the Californian Institute for Regenerative Medicine. Trounson is currently a Distinguished Scientist at the Hudson Institute of Medical Research. He was made an Officer of the Order of Australia in 2021.
A/Prof John Leeton AM
John Leeton was a gynaecologist and obstetrician who held various appointments at Monash University from 1964. He established Melbourne's first comprehensive family planning clinic in 1967 and the first donor sperm program in 1974. In 1971, he founded the first clinical IVF program at Monash University and was its clinical director until 1984, as well as Director of the Monash IVF donor egg program. From 1968-1987, Leeton was Director of the infertility clinic at the Queen Victoria Medical Centre in Melbourne. He was made a Member of the Order of Australia for service to medicine in 2002.
Ian Johnston AM
Ian Johnston (1930-2001) was Head of the Reproductive Biology Unit at the Royal Women’s Hospital. In this role he introduced the use of laparoscopy to diagnose abnormalities that cause infertility. In 1982, he was the founding President of the Fertility Society of Australia and was responsible for introducing support and counselling services for patients and families. In 1997, Johnston established the first Australian workshop on artificial insemination by donor sperm. He was made a Member of the Order of Australia for service to medicine in 2001.
Prof Henry Sathananthan
Henry Sathananthan (1934-2016) was a world-leading electron microscopist who published extensively in the major reproductive science journals. His observations of human sperm, eggs and embryos led to key developments in IVF technologies. Educated in Sri Lanka and England, Sathananthan was Associate Professor at La Trobe University from 1976 to 1998. In 1980, he became a member of the clinical IVF team at Monash University. In 1998, Sathananthan was appointed Honorary Professor at Monash University.
Cryopreservation
Initially, IVF involved the transfer of multiple embryos to the mother’s uterus, as this increased the likelihood of embryo uptake and pregnancy. However, this approach also increased likelihood of multiple pregnancies and the accompanying risks for both mother and child, including miscarriage, premature birth, birth defects and stillbirth. Using cryopreservation, embryos were implanted one at a time and, if the first cycle did not result in a pregnancy, patients could transfer frozen embryos from their previous cycle and were spared the discomfort of additional cycles of egg collection.
References
This case study was developed with input from Professor Alan Trounson, Associate Professor John Leeton and in partnership with Monash University.
The information and images from which impact case studies are produced may be obtained from a number of sources including our case study partner, NHMRC’s internal records and publicly available materials.
The following sources are referenced in this case study:
- Herbert D, Lucke J, Dobson A. Infertility in Australia circa 1980: an historical population perspective on the uptake o f fertility treatment by Australian women born in 1946-51. Australian and New Zealand Journal of Public Health. 2009;33(6):507-514.
- Higgins D. Past and present adoptions in Australia. Melbourne: Australian Institute of Family Studies; 2012.
- Yanagimachi R. M.C. Chang: a pioneer of mammalian in vitro fertilization. Molecular Reproduction and Fertility. 2016;83(10):846-849.
- What is infertility? [Internet]. IVF Australia. 2022. Available from: https://www.ivf.com.au/planning-for-pregnancy/what-is-infertility
- AIHW, Dean J, Sullivan E. Assisted conception Australia and New Zealand 2000 and 2001. Canberra: Australian Institute of Health and Welfare; 2003.
The following additional sources were consulted for this case study:
- Alafaci A. Biographical entry: Johnston, Walter Ian Harewood (Ian) (1930 - 2001) AM, FRCOG, FRACOG. Encyclopedia of Australian Science. [Internet]; 2011. Available from: https://www.eoas.info/biogs/P004805b.htm
- Alafaci A. Biographical entry: Leeton, John FRCOG, FRACS, FRACOG. Encyclopedia of Australian Science. [Internet]; 2007. Available from: https://www.eoas.info/biogs/P004779b.htm
- Cohen J, Trounson A, Dawson K, Jones H, Hazekamp J, Nygren K et al. The early days of IVF outside the UK. Human Reproduction Update. 2005;11(5):439-460.
- Cox L. The development of infertility treatment in Australia. Australian and New Zealand Journal of Obstetrics and Gynaecology. 1991;31(3):254-9.
- Johnston I, Lopata A, Speirs A, Hoult I, Kellow G, Plessis Y. In vitro fertilization: The challenge of the eighties. Fertility and Sterility. 1981;36(6):699-706.
- Kovacs G. Tales from the test tube revolution. O&G Magazine. 2016;(18.1).
- Leeton J. The early history of IVF in Australia and its contribution to the world (1970-1990). The Australian and New Zealand Journal of Obstetrics and Gynaecology. 2004;44(6):495-501.
- Melbourne IVF. 30th Anniversary of IVF in Australia [Internet]. 2010. Available from: https://www.mivf.com.au/about-melbourne-ivf/ media-releases/30th-anniversary-of-ivf-in-australia
- National Health and Medical Research Council. Ethical guidelines on the use of assisted reproductive technology in clinical practice and research. Canberra: National Health and Medical Research Council; 2017.
- Richmond C. Carl Wood obituary. The Guardian [Internet]. 2011. Available from: https://www.theguardian.com/science/2011/oct/16/ carl-wood-obituary
- Trounson A. Obituary: Henry Arunachalam Sathananthan (1934-2016). Reproductive BioMedicine Online. 2017;34(6):555.
- Trounson A. Development of IVF in Australia. Fertility and Sterility. 2018;110:19-24.
- Tuoti W. History of the Monash IVF Research Program from 1971 to 1989 [Internet]. The Embryo Project Encyclopedia. 2020. Available from: https://embryo.asu.edu/pages/history-monash-ivf-research-program-1971-1989
Partners
