Aboriginal and Torres Strait Islander health evidence-practice policy gap reports. An evidence-practice/policy gap is the difference between what is known from the best available research evidence and what is practised in reality (through delivery of medical care or drafting of policies or guidelines).
Publication Data
The identification and reporting of evidence-practice/policy gaps is consistent with the overarching aims of the National Health and Medical Research Council (NHMRC), as defined in the National Health and Medical Research Council Act 1992:
- To raise the standard of individual and public health throughout Australia
- To foster the development of consistent health standards between the various states and territories
- To foster medical research and training and public health research and training throughout Australia
- To foster consideration of ethical issues relating to health.
Identifying and exploring evidence-practice/policy gaps will facilitate more effective allocation of funding to areas of greatest need and raise awareness of the extent of these gaps to encourage the development of more effective health services, guidelines and policies.
The evidence-practice/policy gaps project began in 2015 as a means of showcasing the impact to date (and identifying areas for improvement) of NHMRC funding of Aboriginal and Torres Strait Islander research.
Aboriginal and Torres Strait Islander health
| Influenza vaccination of Aboriginal and Torres Strait Islander adults | 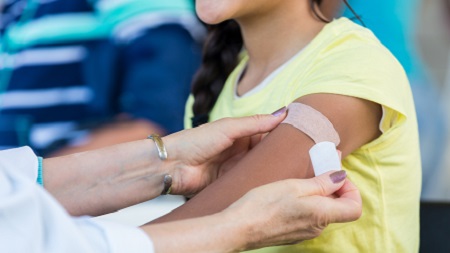 | Current influenza vaccination coverage in Indigenous Australian adults is 34 per cent. Increasing the coverage to 90 per cent would prevent 1,200 hospitalisations and 250 deaths in Indigenous adults each year. Although free annual influenza vaccinations are available, the uptake is low. Better community consultations and engagement are required to ensure higher vaccination rates. |
|---|---|---|
| Evidence-based management of otitis media in high risk populations. | %20with%20Jessica%20Young_RDH3141.JPG) | Ear infections have a significant impact on Aboriginal and Torres Strait Islander children, frequently leading to hearing loss and putting them at an educational disadvantage. Clinical guidelines highlight the need for regular ear checks at doctor appointments, and better training for health professionals to recognise and treat ear disease. Better ear health means better hearing and improved learning, behaviour and school attendance, leading to better educational opportunities and social outcomes for future generations. |
| Delivering family-centred care for Aboriginal and Torres Strait Islander children aged < 5 years |  | Family-centred care is not being fully delivered across primary healthcare services particularly in child health. While the delivery of services has improved, follow-up health assessment still remains poor. Family oriented care could improve the health and wellbeing of Aboriginal and/or Torres Strait Islander children and their families by empowering families to make informed decisions, supporting a holistic concept of care for young children and their families. |
| Culturally safe advice on alcohol cessation in pregnancy |  | Health professionals are well-positioned to prevent Fetal Alcohol Spectrum Disorder (FASD) through providing accurate and timely advice about risks, complications and referral services. However, gaps exist in their knowledge, skills and confidence, particularly within Aboriginal and Torres Strait Islander Australian communities. Properly trained health professionals will better ensure women are informed that no alcohol is the safest option when pregnant. This will also ensure women who are alcohol addicted have increased access to support and treatment services. |
| Early diagnosis of Fetal Alcohol Spectrum Disorder in Indigenous children |  | Guidance and training for health professionals to recognise the signs of Fetal Alcohol Spectrum Disorder (FASD) and treatment options for Indigenous children will mean earlier diagnosis and treatment. Early diagnosis can reduce rates of intellectual disabilities, behavioural and developmental disorders. These improvements will reduce the burden to health care, education and justice systems. |
The aims of these reports are to:
- Take advantage of NHMRC’s legislated role to provide advice to governments and the community,
- Demonstrate how adopting the findings of research could lead to improved health outcomes,
- Demonstrate the impact of NHMRC funding,
- Raise awareness, celebrate success, acknowledge where there is room for improvement (such as care delivered in a manner that is not consistent with the best available evidence), and identify research that will address the gap, and
- Direct funding of Aboriginal and Torres Strait Islander research to areas of greatest need.
Background
In 2002, the NHMRC pledged to allocate a minimum of 5% of the total Medical Research Endowment Account each year to fund research in Aboriginal and Torres Strait Islander health, which has been achieved since 2008. The Principal Committee Indigenous Caucus (PCIC) identified research translation in Indigenous health as a priority in 2012. To demonstrate the impact of the 5% pledge, as well as highlight areas for further improvement, the NHMRC proposed a body of work in 2015 relating to research translation in Indigenous health.
The NHMRC Translating Research into Policy and Practice (TRIPP) Forum held in May 2016 identified the most significant current evidence-practice/policy gaps, and sorted these according to the Life Course stages (obtained from the National Aboriginal and Torres Strait Islander Health Plan 2013-2023). Additional gaps were identified from financial data from NHMRC and input from PCIC. The NHMRC identified authors for evidence-practice/policy gap synopses for the report from relevant national Centres of Research Excellence (CREs). Synopses were peer reviewed by a member of PCIC and external referees.
Achievements to date include:
- An overview of systematic reviews of research into the health of Aboriginal and Torres Strait Islander peoples
- A Special Collection of the Cochrane Library: Health of Indigenous Peoples
- A forum to identify current evidence-practice/policy gaps, held in 2016: Translating Research Into Policy and Practice (TRIPP) forum
NHMRC acknowledges the time and effort, and express our genuine gratitude for the contributions and support of the peer reviewers.