Road Map 3: A strategic framework for improving Aboriginal and Torres Strait Islander health through research.
Linked to:
Publication Data
Table of contents
About NHMRC
The National Health and Medical Research Council (NHMRC) has been the Australian Government body for supporting health and medical research since 1937. The overall purposes of NHMRC, supporting the agency's mission of 'working to build a healthy Australia', can be summarised as follows:
- fund high quality health and medical research and build research capability
- support the translation of health and medical research into better health outcomes
- promote the highest ethical standards in health and medical research.
Our commitment to improving Aboriginal and Torres Strait Islander health outcomes covers all aspects of NHMRC's principal functions: pursuing activities which raise the standard of individual and public health throughout Australia, fostering the development of consistent health standards between the states and territories, supporting medical and public health research and training and promoting consideration of ethical issues related to health.
This commitment to improving the health of Aboriginal peoples and Torres Strait Islander peoples through the support of health research and its translation is set out as a priority in our annual Corporate Plan. Further details on strategies to strengthen the Aboriginal and Torres Strait Islander health sector and identify priority health research topics are documented in our Road Maps.
While we celebrate the achievements of Road Maps 1 and 2 and the investment to date in Aboriginal and Torres Strait Islander health and medical research, we also recognise the opportunities to further strengthen research processes, the research workforce and ultimately health outcomes for Aboriginal and Torres Strait Islander peoples and communities.
1 Foreword
Our strategic vision for Aboriginal and Torres Strait Islander health and medical research
The National Health and Medical Research Council (NHMRC), advised by and in collaboration with its Principal Committee Indigenous Caucus (PCIC), is pleased to present Road Map 3 to provide NHMRC’s strategic direction for Aboriginal and Torres Strait Islander health and medical research over the next ten years.
Road Map 3 is the product of an extensive consultation process in which researchers, health workers, government officials and community members came together to advise on the future direction for research. In that sense, Road Map 3 belongs to the whole community who have shared their insights and passions for improving Aboriginal and Torres Strait Islander health outcomes.
NHMRC has achieved its target of 5% of total research funding being allocated to Aboriginal and Torres Strait Islander health and medical research since 2008. In 2017, 6.2% of funding or $49.7 million was allocated which is a solid achievement. NHMRC remains committed to supporting the highest quality research that drives improvements in health outcomes for Aboriginal and Torres Strait Islander peoples and communities.
Road Maps 1 and 2 have provided a foundation on which to build. We demonstrate our ongoing commitment to supporting and enabling health and medical research for and by Aboriginal and Torres Strait Islander Australians through the development of Road Map 3.
Road Map 3 is intended for a broad audience of researchers, policy makers and community members. We hope that Road Map 3 provides a clear direction for the foreseeable future, a future in which Aboriginal and Torres Strait Islander peoples and communities are strong owners, participants and beneficiaries of research at all levels.
2 Introducing Road Map 3
Background and context
Road Map 3 is a strategic framework that draws on the deep understanding of Aboriginal and Torres Strait Islander health and medical research contributed by researchers, health workers, government officials and community leaders during an extensive consultation process1. This process involved seven workshops across the country and nine dialogues with leaders and experts in the field. During the course of the consultation process the context and priorities for Road Map 3 were considered and developed with a firm focus on the desired outcome – that research funded by NHMRC over the next 10 years provides the best value and impact in improving health outcomes for Aboriginal and Torres Strait Islander peoples and communities.
Road Map 3 contains a number of priorities that relate to NHMRC processes and investments in the Aboriginal and Torres Strait Islander health research workforce; and engagement and consultation with Aboriginal and Torres Strait Islander communities, as well as particular research focus areas. Road Map 3 draws on the key themes that emerged from the consultation process. These included that Road Map 3 should:
- recognise the evolving context within which it is framed
- build on the fundamental concepts of Road Maps 1 and 2
- support Aboriginal and Torres Strait Islander representation and leadership in NHMRC's
- processes and structures
- address the challenge of measuring effort and impact.
Road Map 3 recognises the evolving context within which it is framed
The structures within which NHMRC will determine its funding allocations over the foreseeable future are changing with the implementation of the new grant program. NHMRC remains committed to the target set in Road Maps 1 and 2 of a 5% allocation of the overall Medical Research Endowment Account to Aboriginal and Torres Strait Islander health and medical research.2
Change is also occurring externally to NHMRC. The critical need for improved health outcomes for Aboriginal and Torres Strait Islander peoples continues to gain prominence in Australia and overseas. Recognition of institutional racism is also growing as a factor that impacts on health service delivery. Road Map 3 seeks to allow these concepts to guide how health and medical research can improve Aboriginal and Torres Strait Islander peoples' health.
Road Map 3 builds on the fundamental concepts of Road Maps 1 and 2
Road Maps 1 and 2 were published in 2002 and 2010 respectively. Road Map 3 follows and builds on both these documents. The Road Map 3 consultation process emphasised the importance of health as a holistic concept, based on the World Health Organisation (WHO) definition of wellness3 and the National Aboriginal Health Strategy4 definition of Aboriginal health.

(Quotes in image: 'Health is a state of complete physical, mental and social well-being and not merely the absence of disease or infirmity.' WHO'Aboriginal health means not just the physical well-being of the individual but refers to the social, emotional and cultural well-being of the whole community. This is a whole of life view and included the cyclical concept of life-death-life.' National Aboriginal Health Strategy, 1989.)
The consultations also reiterated the ongoing importance of research into the social and cultural determinants of health as well as health system, service delivery and translational research. Issues that fall more into the category of 'public health' rather than medical advances were viewed as particularly important. There was also a recognition that advances in fields related to genomics and other developments in basic biology and personalised medicine will be increasingly critical to the improvement of health care outcomes for Aboriginal and Torres Strait Islander peoples and communities.5
Some specific concepts remain pivotal and unchanged in Road Map 3. Community engagement as an integral part of high quality research is fundamental to Road Maps 1, 2 and 3, as is the need to foster a larger cohort of Aboriginal and Torres Strait Islander researchers at all levels. Throughout the Road Map 3 consultation process, the importance of these concepts was agreed to by all. Ideas and discussions focused on how to best achieve each of these fundamental goals.
Road Map 3 supports Aboriginal and Torres Strait Islander representation and leadership in NHMRC's processes and structures
The approach that NHMRC has adopted to ensure there is Aboriginal and Torres Strait Islander participation on each of its committees, and the formation of the Principal Committee Indigenous Caucus (PCIC), is valued by the research community. Under the leadership of the PCIC, the ongoing development of guidance material, research protocols and criteria to underpin Aboriginal and Torres Strait Islander health and medical research (such as ethics guidance and the Indigenous Research Excellence Criteria) provides a critical backdrop to the future directions outlined in Road Map 3.
Road Map 3 addresses the challenge of measuring effort and impact
Commitments in Road Maps 1 and 2 to measure the research effort and the impact of funded research were not clearly aligned with outcomes. Clear and more regular accountability and reporting on the research funding allocated to Aboriginal and Torres Strait Islander research under Road Map 3 was a consistent message during the consultation process.
To assist in the development of Road Map 3, NHMRC reported on the extent and nature of Aboriginal and Torres Strait Islander health and medical research and achievements to date. This demonstrated that in 2016, 6.3% of the total NHMRC investment was allocated to research grants that had an Aboriginal and Torres Strait Islander health research focus or was conducted by an Aboriginal and/or Torres Strait Islander researcher.6
Other NHMRC achievements include:

3 Setting our objective for Road Map 3

(Text in image: The overall objective of Road Map 3 is to: guide NHMRC to improve health, social and wellbeing outcomes for Aboriginal and Torres Strait Islander peoples by ensuring research excellence and integrity - highlighting research priorities driven by Aboriginal and Torres Strait Islander communities.)
The following interrelated components will play an important role in achieving the objective
of Road Map 3:
- Focus on research that makes a difference — a successful Road Map 3 will guide research investments that lead to benefits for Aboriginal and Torres Strait Islander peoples and communities. This means that the proposed research areas must reflect national health priorities and health issues identified as important by Aboriginal and Torres Strait Islander peoples and communities. An essential part of identifying and conducting research that will improve health outcomes for Aboriginal and Torres Strait Islander peoples and communities is to ensure that health and medical research embodies an Aboriginal and Torres Strait Islander definition of health that reflects holistic wellbeing and collective approaches.
- Research excellence and integrity — integrity refers to both the quality of research and the process by which research is undertaken. Research excellence is influenced by factors such as a researcher’s track record and their relevant experience in a particular health topic area. Track record is broader than academic research outputs and includes the health, social, economic and knowledge impact of research, as well as leadership in the research and broader community. The research team composition and level of Aboriginal and Torres Strait Islander involvement in, and particularly leadership of, the project are also important. For Road Map 3 to be successful, adhering to NHMRC ethical protocols and guidelines must be at the core of all research projects. This will ensure that the research benefits Aboriginal and Torres Strait Islander peoples and communities.
- Strong community engagement — community consultation has been a driving force for the development of all NHMRC Road Maps. This must also flow through to the different stages of the grant application and research process so that researchers from all backgrounds are supported to meaningfully engage with Aboriginal and Torres Strait Islander peoples, communities and organisations. Through appropriate and ethical consultation and partnership arrangements, researchers will better identify and deliver projects that translate into benefits and health improvements.
4 Focusing on our delivery: Road Map 3 priorities
Road Map 3 has a focus on three priority areas:

While Road Map 3 provides a ten year plan, NHMRC acknowledges the importance of reflecting on progress towards targets and considering opportunities for continual improvement. Every three years, NHMRC will produce an Action Plan, which will present the focus areas and targets for the coming triennium and report on key achievements from the previous triennium. This time horizon will be in line with trienniums for new committees and NHMRC's strategic plan. More information on the Action Plan can be found in Section 5.
4.1 Strengthen the Aboriginal and Torres Strait Islander researcher workforce
NHMRC is strongly committed to supporting the development of Aboriginal and Torres Strait Islander health and medical researchers. NHMRC will continue its investment in building the research workforce through the following initiatives:
- Building workforce capacity in the sector — NHMRC will support Aboriginal and Torres Strait Islander early career researchers to realise opportunities to become leaders in the Aboriginal and Torres Strait Islander health and medical research sector.
- Supporting community based researchers — NHMRC will explore how it can support researchers who develop research expertise from non‑traditional pathways. Health policy, translation and research dissemination are all factors that contribute to track record. There are opportunities for non‑academic researchers, including those who work in the community controlled sector to participate in research and work closely with professional peak bodies.
- Monitoring Aboriginal and Torres Strait Islander researchers’ participation in NHMRC programs — NHMRC will actively monitor and report on participation by Aboriginal and Torres Strait Islander researchers in NHMRC funded programs. This includes monitoring and reporting on numbers of individuals receiving grants as a Chief Investigator and participating in other ways in NHMRC-funded research.
These key action areas will be supported by a series of initiatives that will be released as part of the three-year Action Plans. Monitoring and reporting will help track progress against initiatives in key action areas.
NHMRC's role will build on the efforts of other research bodies and organisations that support the Aboriginal and Torres Strait Islander health research sector and Aboriginal and Torres Strait Islander researchers. This includes universities that have a responsibility for developing early career Aboriginal and Torres Strait Islander researchers and peak body organisations that have a predominant focus on Aboriginal and Torres Strait Islander health.
4.2 Engage with Aboriginal and Torres Strait Islander communities
NHMRC is strongly committed to ensuring meaningful engagement with Aboriginal and Torres Strait Islander communities. NHMRC will continue to enhance its engagement with communities in the following ways:
- Actively engage with communities to identify health and medical research priorities — NHMRC will provide opportunities for communities to provide input on key research priorities through regular consultation on Aboriginal and Torres Strait Islander health and medical research priorities. Targeted Calls for Research will support this process by providing community‑identified research priorities for health researchers to pursue.
- Continuing to recognise PCIC as the major advisory body to NHMRC on Aboriginal and Torres Strait Islander health research — This includes expanding the remit of the PCIC to include monitoring and review of progress against key milestones relating to Road Map 3.
- Supporting researchers to engage strongly and effectively with communities — Excellent research means researchers need to account for their engagement with Aboriginal and Torres Strait Islander communities throughout the research project lifecycle, from planning to communicating outcomes with an emphasis on translation. NHMRC will strongly encourage this project lifecycle engagement in its research applications through the Indigenous Research Excellence Criteria. NHMRC funding timeframes will also seek to provide appropriate lead times for researchers to engage with communities.
- Continually improving key protocol documents and guidelines — NHMRC, with advice from PCIC, will review existing protocols and guidelines that relate to research with Aboriginal and Torres Strait Islander communities. This will include reviewing the Indigenous Research Excellence Criteria.
NHMRC strongly encourages any research with Aboriginal and Torres Strait Islander peoples to observe the Values and Ethics: Guidelines for Ethical Conduct in Aboriginal and Torres Strait Islander Health Research and the Keeping Research on Track: A guide for Aboriginal and Torres Strait Islander peoples about health research ethics documents.
NHMRC will also develop and implement an Indigenous Engagement Strategy. This will be an internal document which will guide engagement with Aboriginal and Torres Strait Islander peoples, communities and organisations.
4.3 Support research in high priority areas
Road Map 3 identifies the most important areas of focus to benefit Aboriginal and Torres Strait Islander health outcomes. The priority research areas have been grouped into three categories that together represent research that is likely to result in the greatest value and outcome to benefit Aboriginal and Torres Strait Islander peoples and communities.
The three categories are:

(Text in image: 3 categories are (1) Research that is focused on the health system and the social and cultural determinants of health for Aboriginal and Torres Strait Islander peoples and communities (2) Research areas where there is a significant burden of disease and/or the highest differential quality of life in Aboriginal and Torres Strait Islander communities (3) Research on specific diseases that are almost exclusive to Aboriginal and Torres Strait Islander peoples and/or personalised approaches to health care)
1 Research that is focused on the health system and the social and cultural determinants of health for Aboriginal and Torres Strait Islander peoples and communities
Research in this category will have a strong focus on the effectiveness of the health system, and broader social and cultural determinants of health. This includes public health, public policy and disease prevention programs in Aboriginal and Torres Strait Islander communities. Research on the specific health needs and experiences of vulnerable groups within Aboriginal and Torres Strait Islander communities is welcomed. Research on strength-based approaches and knowledge translation is encouraged.
Research under this category is likely to fall into one of the following three areas:
- A focus on particular life stages, such as childhood, adolescence and ageing
- A focus on applied research, that identifies community strengths and can be leveraged for wellbeing improvement
- An assessment of the appropriateness and effectiveness of health systems and services for Aboriginal and Torres Strait Islander peoples and communities.
Examples of specific research topics that would fall within this category include:
- social determinants of health – such as poverty, housing and education
- the effectiveness of the health system for Aboriginal and Torres Strait Islander peoples and communities
- cultural competence, cultural safety and racism in the health system
- maternal and adolescent health
- healthy ageing
- diet and nutrition and public health and preventative disease programs
- culture and its relationship with Aboriginal and Torres Strait Islander health
- prevention.
2 Research areas where there is a significant burden of disease and/or the highest differential quality of life in Aboriginal and Torres Strait Islander communities
The second category has a greater focus on applied and translational research ensuring that the research has the greatest impact on Aboriginal and Torres Strait Islander health outcomes. Research that falls into this category would have one or more of the following attributes:
- A focus on improving Aboriginal and Torres Strait Islander health outcomes
- A focus on applied research and translation of research into health outcomes in Aboriginal and Torres Strait Islander communities or in a health setting for Aboriginal and Torres Strait Islander peoples, including health system improvement research, public policy research, implementation
- research and program evaluation research
- A focus on major burdens of disease and death for Aboriginal and Torres Strait Islander peoples and/or conditions that have a significant impact on quality of life.
- Examples of specific research topics that would fall within this category include:
- social and emotional wellbeing and mental health conditions, including dementia
- chronic physical health conditions, including cancer, diabetes, kidney health and respiratory and cardiovascular diseases
- intervention research in other communities that could be applied to an Aboriginal and/or Torres Strait Islander setting or context.
3 Research on specific diseases that are almost exclusive to Aboriginal and Torres Strait Islander peoples and/or personalised approaches to health care
The third research category focuses on diseases that are almost exclusive to Aboriginal and Torres Strait Islander communities, as well as personalised approaches to healthcare through developments in genomics and other fields.
Research that falls within this category will have one or more of the following attributes:
- A focus on diseases and other health issues that are largely specific to or almost exclusive to Aboriginal and Torres Islander communities or research that is focused on personalised approaches to healthcare for Aboriginal and/or Torres Strait Islander peoples
- A focus on topics that span the spectrum of health research—basic science, public health, clinical medicine and science, and health services research.
Examples of specific research topics that would fall within this category include:
- rheumatic heart disease
- eye and ear health
- certain vector borne infectious diseases, particularly in the Torres Strait
- acute renal failure
- other emerging diseases in Aboriginal and Torres Strait Islander communities
- genomics and personalised approaches to healthcare for mainstream diseases.
4.4 Priorities will differ over time and for different Aboriginal and Torres Strait Islander communities
The three priority research categories identified above provide an indication of the types of research that may be funded under each category. It should be noted that research priorities across distinct Aboriginal and Torres Strait Islander communities will likely differ. For this reason, researchers will need to work closely with Aboriginal and Torres Strait Islander peoples and communities to understand what research is important to individual communities. Similarly, research priorities may change and develop over time, therefore specific research priorities used as examples above provide guidance only.
The Road Map 3 Action Plan will provide information on emerging research priorities within the three categories highlighted here. In addition to this, Targeted Calls for Research will also address emerging research issues in Aboriginal and Torres Strait Islander health that have not been identified previously, or that have been highlighted as key concerns or urgent areas requiring attention. Targeted Calls for Research will stimulate or greatly advance research in a particular area of health and medical science that will benefit the health of Australians, complementing NHMRC's existing suite of funding schemes by funding priority research in defined areas of need and when urgent research needs emerge.
5 Monitoring our progress: Road Map 3 review and reporting
NHMRC is committed to transparency and accountability through tracking progress against a set of targets and key performance indicators set out in an Action Plan. The PCIC will monitor progress, and provide guidance and direction on strengthening Road Map 3's approach and outcomes.
An annual Report Card will communicate progress against Road Map 3 Action Plan to stakeholders.
Road Map 3 Action Plans and Report Cards will be made available on NHMRC's website.
Appendix A: Development of Road Map 3
Road Map 3 has been developed in collaboration with NHMRC, PCIC and key stakeholders involved in Aboriginal and Torres Strait Islander health research and researchers. The consultation processes, which began in March 2017, engaged stakeholders to:
- consider what has changed in the context of Aboriginal and Torres Strait Islander health and medical research and health outcomes since the release of Road Map 1
- think critically about the strengths and achievements of Road Maps 1 and 2, as well as the opportunities for improvement
- test and refine the objective for Road Map 3
- discuss ideas for research priority areas for Road Map 3
- generate insights on how NHMRC can continue to engage with Aboriginal and Torres Strait Islander communities and health researchers and strengthen the Aboriginal and Torres Strait Islander health research sector.
The process involved ongoing dialogue with Aboriginal and Torres Strait Islander health and research peak bodies and seven workshops across Australia. For those who could not attend the workshops, there was an opportunity to provide input or feedback via an online survey.
The consultation process ended with an opportunity for the general public to provide written submissions to NHMRC. The online public consultation process was held from July to December 2017. A total of 21 submissions were received from individuals and organisation. Figure 1 below provides an overview of the consultations. A report on the outcomes of the consultation process can be found here.
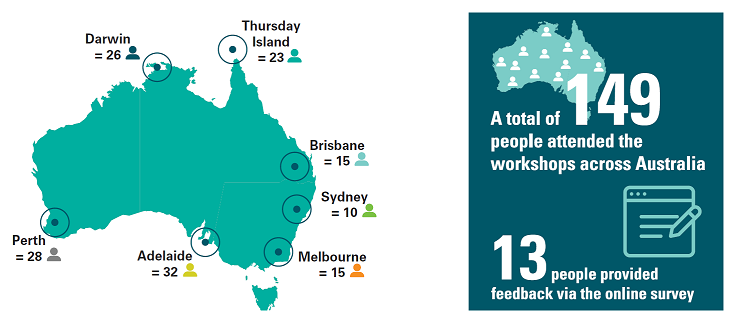
(Text in image: A total of 149 people attended the workshops across Australia.13 people provided feedback via the online survey. Darwin = 26, Thursday Island = 23, Brisbane = 15, Sydney = 10, Melbourne = 15, Adelaide = 32, Perth = 28.)
Footnotes
1 The consultation process and the themes which emerged are set out in the compendium document, Road Map 3: A strategic framework for improving Aboriginal and Torres Strait Islander health through research: Report of Community Consultations
2 NHMRC has a commitment to spend at least 5% of funding under the Medical Research Endowment Account on Aboriginal and Torres Strait Islander health research each year; NHMRC (2017), accessed online, available at Aboriginal and Torres Strait Islander health
3 World Health Organisation (2017), Constitution of WHO principles, accessed online 1 August 2017, available at: https://www.who.int/about/governance/constitution
4 This is the definition of 'Aboriginal health' as outlined in the 1989 National Aboriginal Health Strategy, as included in the NACCHO Constitution. Accessed online 1 August 2017, available at: https://www.naccho.org.au/acchos/
5 This topic area is also identified as important in the National Research Infrastructure Roadmap. Australian Government (2016), National Research Infrastructure Road Map, Australian Government, accessed online 18 July 2017, available at https://www.chiefscientist.gov.au/sites/default/files/ED16-0269-National-Research-Infrastructure-Roadmap-Report_Internals_ACC.pdf_infrastructure_roadmap_report_internals_acc.pdf, pg 34.
6 To qualify as Aboriginal and/or Torres Strait Islander health research, NHMRC Funding Rules state that "at least 20% of the research effort and/or capacity building must relate to Aboriginal and/or Torres Strait Islander health."