Developed through collaboration with Aboriginal communities, the Kimberley Mum’s Mood Scale (KMMS) improves early detection of mental health and social, emotional and cultural wellbeing concerns and promotes culturally safe care for Aboriginal and Torres Strait Islander women. Its adoption in routine primary health care illustrates the enduring impact of community driven research.
Aboriginal and Torres Strait Islander women are strong and resilient. However, the ongoing impacts of colonisation, racism, trauma, and social and structural inequities have led to significant disparities in perinatal mental health outcomes. Improving the early detection and treatment of perinatal mental health concerns among Aboriginal and Torres Strait Islander women is recognised as a national priority.
In the Kimberley region, concerns were raised that the Edinburgh Postnatal Depression Scale (EPDS) was not the most suitable tool for engaging and screening Aboriginal and Torres Strait Islander women. In response, a community based research project was undertaken to explore more culturally appropriate approaches to perinatal mental health screening. More than 100 Kimberley Aboriginal women and 72 healthcare professionals contributed to this process.

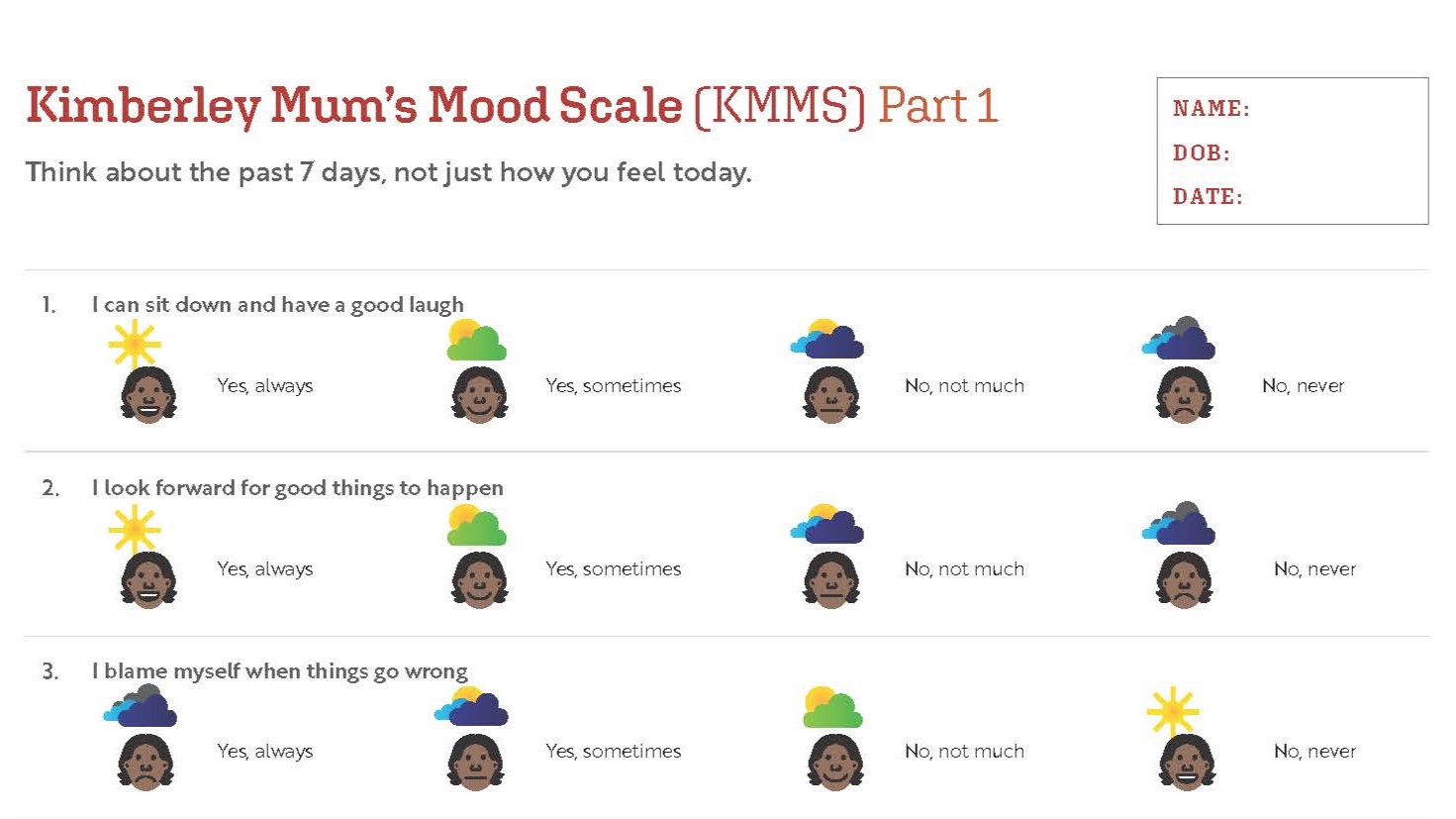
This collaboration resulted in the development of the Kimberley Mum’s Mood Scale (KMMS), a 2-part screening tool. Part one is a modified version of the EPDS, while part 2 uses a yarning based template to explore psychosocial areas of stress and resilience in a woman’s life.
“The development of the KMMS was driven by the need for a screening tool that centres the voices and experiences of Aboriginal women,” said Professor David Atkinson.
The KMMS was validated in a clinical trial involving 91 Aboriginal women in the Kimberley region. The study found that the KMMS effectively identified women experiencing moderate to severe depression or anxiety. It was also found to be acceptable and culturally appropriate for Aboriginal women and their healthcare providers.

Professors David Atkinson and Julia Marley from The University of Western Australia’s Rural Clinical School of Western Australia worked in close partnership with the Kimberley Aboriginal Medical Services, Apunipima Cape York Health Council and the Western Australian Country Health Service to build on the success of the KMMS. Together they submitted a NHMRC Partnership Grant application to ensure the tool could be implemented and embedded into routine primary health care practice across the Kimberley. The grant also aimed to explore the acceptability of the KMMS in other geographical locations.
“The KMMS was well received by both community members and healthcare providers, but NHMRC funding was needed to support sustained implementation,” said Professor Marley.
Upon successfully receiving NHMRC funding, Bardi Jawi researcher, Erica Spry ‘Roobaanjarn’, and early career researcher, Dr Emma Carlin, joined the team, further strengthening the project’s community leadership and research capacity. Acceptability studies were undertaken in Pilbara in Western Australia, Cape York in Queensland, and Gove in the Northern Territory to explore how the KMMS works in different regional and cultural contexts. These studies aimed to understand the experiences of Aboriginal women, health professionals, and community stakeholders in using the KMMS, assessing its cultural relevance, usability, and fit within local models of care.
“We wanted to reinforce that the KMMS assesses not only risk but also protective factors. By engaging with the mother, exploring her strengths through clinical yarning and building her confidence, screening becomes culturally safe. We move past the deficit discourse and work in partnership with the mother to understand and support her wellbeing,” said Ms Spry.
The KMMS team has since focused on translating research into real world practice by embedding the KMMS into routine primary health care in ways that can be sustained and are culturally safe. This included developing free online training through Emerging Minds and NACCHO Learn, integrating the tool into various electronic medical record systems, and making it available on the iCOPE digital screening platform so it can be used across diverse health services.
The KMMS has been formally recognised in the NHMRC-led Living Guidelines and the NACCHO RACGP Preventative Health Guide. It has been adopted by the Kimberley Aboriginal Health Planning Forum and forms the basis of the region’s Perinatal Depression and Anxiety Protocol. The KMMS has also been adopted by jurisdictions within state and territory health departments. This broad endorsement demonstrates that culturally secure approaches can lead the way in evidence based care.
Health professionals have reported that the tool strengthens culturally safe practice and builds confidence in providing mental health care. The lessons from these studies are helping refine implementation approaches and to ensure the KMMS remains responsive to the unique needs and strengths of Aboriginal and Torres Strait Islander communities across Australia.
“We continue to find that the KMMS helps create a safe space for Aboriginal women to share their experiences and for health professionals to listen and respond in safe and meaningful ways,” said Dr Carlin.
Working in partnership with Aboriginal people and communities, Aboriginal Community Controlled Health Organisations, and state based health services has been at the heart of the KMMS journey. This collaboration continues to demonstrate how Aboriginal leadership, community partnerships, and culturally grounded research can transform perinatal mental health care across Australia.
Next steps
The next phase of work will focus on supporting broader use of the KMMS across Australia to strengthen early and culturally safe identification of perinatal depression and anxiety. There is interest in exploring the acceptability of the KMMS with Torres Strait Islander women to ensure it reflects and respects diverse cultural perspectives and experiences. There is also interest in exploring the acceptability of the KMMS with other First Nations populations to inform potential adaptation and application in Indigenous communities globally.
Chief investigator: Professor David Atkinson, Dr Emma Carlin, Professor Julia Marley and Ms Erica Spry
Administering institution: The University of Western Australia
Team members:
- Dr Catherine Engelke
- Dr Stephanie Trust
- Dr Jaye Kotz
- Ms Katherine Ferrari
- Ms Melissa Williams
- Professor Mark Wenitong
- Professor Karen Edmond
- Professor Ernest Hunter
- Professor Rhonda Marriott
- Professor Yvonne Cadet James
- Ms Jo Neville
- Ms Diana Jans
- Associate Professor Sandra Campbell
- Kimberley Aboriginal Medical Services
- WA Country Health Service
- Mawarnkarra Health Service
- Apunipima Cape York Health Council
- NT Health Department (Gove Hospital)
To the Aboriginal and Torres Strait Islander women who have participated in KMMS research, thank you, without you this work would not exist.
Grant: Partnership Project
Year: 2016–2022
Funding amount: $1,414,104